Innovative Studies Advance Lung Disease Diagnosis and Treatment at ChristianaCare
'Delivering the right care at the right time and doing it better than ever before'
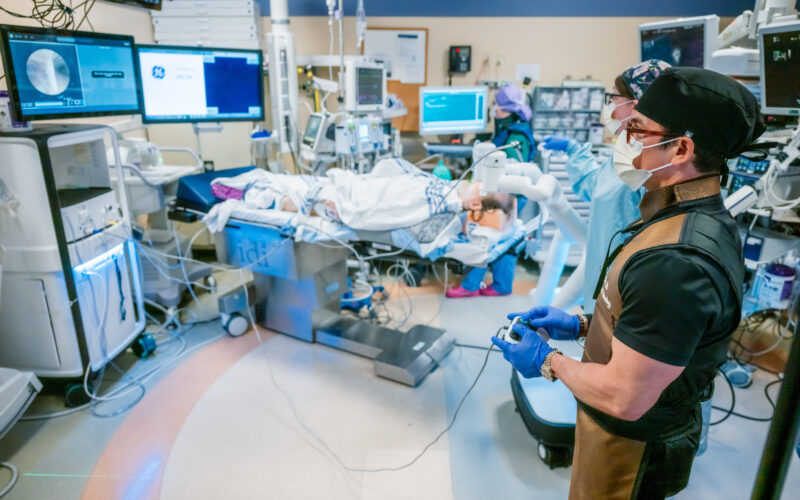
Three new published research studies from ChristianaCare are transforming how lung disease is diagnosed and treated. These studies address critical challenges such as managing cancer-related complications, improving biopsy techniques and strengthening diagnostic safety, while showing how innovation and collaboration can make care safer, more accessible and cost-effective for patients with complex lung conditions.

“Research is the engine that drives progress in cancer care,” said Thomas Schwaab, M.D., Ph.D., Bank of America Endowed Medical Director of ChristianaCare’s Helen F. Graham Cancer Center & Research Institute. “These studies reflect the highest quality science and a deep commitment to improving the lives of our patients.
“At the Graham Cancer Center, we believe that innovation and evidence-based practice are essential to transforming outcomes and setting new standards for excellence.”
Click here for more on Interventional Pulmonology at ChristianaCare.
“These studies show what happens when we combine innovation with collaboration,” said Ismael Matus, M.D., FCCP, lead author on the studies and director of Interventional Pulmonology at ChristianaCare. “By rethinking processes and using technology in smarter ways, we can improve outcomes, reduce costs and make care easier for patients.
“This is about delivering the right care at the right time, and doing it better than ever before.”
Study 1: New Pathway for Treating Malignant Pleural Effusion
Journal of Bronchology & Interventional Pulmonology, January 2026
Malignant pleural effusion (MPE) is a serious complication for people with advanced cancer, often causing pain and breathing difficulties. Traditionally, MPE care involved emergency visits, hospitalizations and multiple specialists.
A new systemwide clinical pathway at ChristianaCare brings together Pulmonology, Surgery, Oncology, Emergency Medicine and Nursing. Electronic medical records enable rapid identification and triage, streamlining care and shifting many treatments to outpatient settings.
Key findings:
- Emergency room visits and hospital stays dropped by more than half.
- Patients needed fewer procedures and saw fewer specialists.
- Average direct cost savings reached $1,145 per patient.
- Streamlined care improved quality of life and system efficiency.
Study 2: Smarter Biopsy Results With Dynamic Cell Imaging
Journal of Bronchology & Interventional Pulmonology, January 2026
Diagnosing lung nodules requires accurate tissue samples. Dynamic Cell Imaging (DCI) allows doctors to check biopsy samples immediately during the procedure, rather than waiting for lab results.
In this study, DCI was used on 50 patients. On-site results matched the pathologist’s diagnosis 88% of the time, giving doctors greater confidence and potentially reducing repeat procedures.
Key findings:
- 88% concordance between on-site DCI and final pathology.
- Fewer repeat procedures and faster answers for patients.
- DCI supports targeted therapies by confirming accurate sampling.
- Demonstrates how existing technology can be repurposed for better care.
Study 3: Ultrasound Instead of X-ray for Safer, Faster Recovery
Journal of Respiration, November 2025
After lung biopsies, chest X-rays are typically used to check for collapsed lung, but they add time, radiation and cost. ChristianaCare researchers evaluated thoracic ultrasound as a replacement.
Key findings:
- In 95.5% of cases, ultrasound alone safely ruled out complications, eliminating the need for routine X-rays.
- Reduced time, radiation exposure and costs.
- Patients discharged sooner, with fewer unnecessary tests.
“When the status quo is challenged and patients are put at the center, safer, faster and more affordable lung care becomes possible. ChristianaCare is committed to leading with innovation and teamwork, because every patient deserves the very best,” said Matus.
ChristianaCare’s pulmonary interventionalists are among the nation’s leading experts in the number of patients they treat, and that experience makes a real difference. Treating a high volume of complex cases builds deep expertise and leads to better outcomes for patients. The team uses advanced, minimally invasive tools like robotic bronchoscopy to diagnose and treat lung and airway conditions with precision. Every patient benefits from personalized care focused on helping them breathe easier and recover faster.