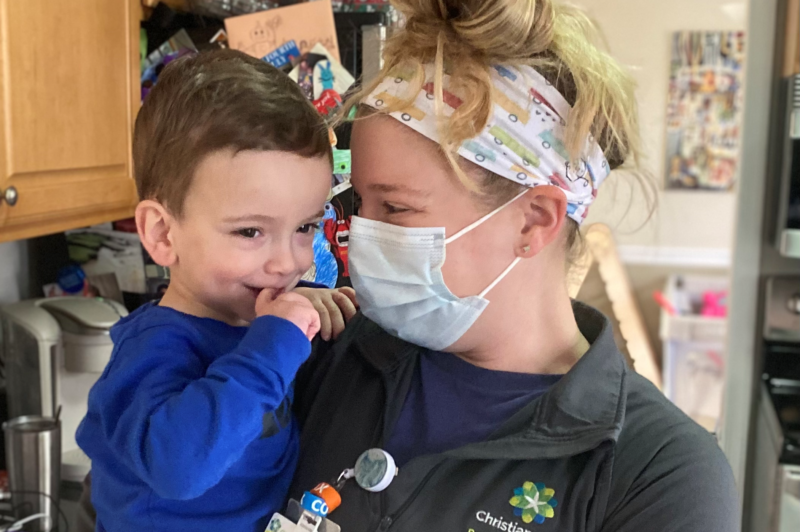
Jen Schulak, MSN, MSM-HCA, RN, NPD-BC, CCRN, steps out of her Pike Creek home with one toddler son burrowed into her shoulder and two more trailing behind her. With her free hand, she pops open a folded stroller wagon. She grabs three bubble wands and three pairs of kid-sized sunglasses.
“All right, Nate, you have to sit. Let’s get you into the wagon.” she says. The other boys, Dylan and Trent, whimper as they wait their turn but Schulak quiets them with a promise: “Don’t worry, I got you next.”
As her 6-year-old son Carter zips past on his scooter, Schulak turns to her husband Jon still standing at the garage door. He’s checking on 3-year-old Brynn, who spilled her bubbles.
“We’re going to do a quick walk and then we’re going to go right back in the house,” Schulak says.
Taking a short family walk with a stroller seemed impossible two years ago, when the young Schulak family grew from four to seven after their identical triplets were born at just 29 weeks. Nate and Dylan spent three months in the ChristianaCare Neonatal Intensive Care Unit (NICU), and their brother Trent stayed for five months.
Supported by expert care, they are now thriving toddlers who sing, climb on furniture and are learning to take turns on their jungle gym.

For Schulak, who works in the Post-Anesthesia Care Unit (PACU) at Christiana Hospital, being on both sides of the patient experience has deepened her gratitude for those who work in health care while continuing to motivate her to pay it forward.
With big brother Carter leading the way, Schulak maneuvers the wagon with her precious cargo down the sidewalk.
“Don’t worry — we’ve got this, right, boys?” she says, grinning.
Sept. 17, 2020
After two relatively uneventful pregnancies — other than going past 40 weeks — Schulak didn’t expect anything out of the ordinary when she arrived for her eight-week ultrasound on Sept. 17, 2020. COVID-19 restrictions limited visitors to patient appointments, so she went alone on her lunch break. Before the scan, she and her obstetrician, Alexander Kirifides, D.O., joked about her having twins.

“The moment he turned on the sound, I could hear something different. I was a little nervous thinking something was wrong. He said, ‘No, Jen, there’s not just two, There’s three,’” she said.
“He kept asking me, ‘Are you sure you’re not on any medication? Is there a family history?’ I told him ‘no, no.’ He said he hadn’t seen a spontaneous triplet pregnancy since residency.”
The odds of conceiving triplets without the use of fertility medication are about one in 10,000 births. But the Schulak triplets were even more unusual – they were monochorionic triamniotic, meaning each fetus had its own amniotic sac but shared one placenta, even more rare at about 1 in 100,000 births.
All of this greatly raised the chances of complications and preterm delivery.
With more than 6,000 babies delivered annually at ChristianaCare – including her two previous children – Schulak knew she was in good hands. But it was an adjustment to go from being the caregiver to being the patient.
With more than 6,000 babies delivered annually at ChristianaCare – including her two previous children – Schulak knew she was in good hands.
“It’s almost surreal. You never think that you’re going to be in that position where you need to seek out care for not only your family, but yourself,” she said.
“But it was such a great experience to be the patient and feel the compassion and the beauty of nursing and medicine,” she said.
“I got to see all the advancements in technology and understand how our caregivers can do what they do so well.”
February 12, 2021
Medical appointments and additional testing soon consumed what little free time the working mom of two had. In addition to her regular obstetric appointments, Schulak was also seen at the Delaware Center for Maternal & Fetal Medicine of ChristianaCare, Inc.

Colleague Alexandra Colin, MSN, RN, CCRN-K, knew her work bestie had a lot on her mind as the months of her pregnancy progressed. They had worked closely as nursing professional development specialists, responsible for over 600 outpatient nursing caregivers. Working with Schulak didn’t feel like work, and that was often because of the way they clicked.
“We faced the challenges together and would find the solutions together,” Colin said. “Even though she’s younger than I am, she inspires me to be like her with her caring self.”
But by her 28th week, Schulak needed to put work on hold. She was hospitalized and on bedrest.

On Feb. 12, 2021, at 29 weeks, she had an emergency C-section because of issues with her placenta.
Dylan, Trent and Nathan were born with 35 caregivers waiting and watching for what these premature triplets might need.
They were quickly taken to the Neonatal Intensive Care Unit (NICU), where they would make their home for the next several months.
Within hours of their births, the Schulaks realized the extent of the challenges their premature sons were facing. All three babies were on ventilators and considered extremely critical.
Three isolettes and attached supportive equipment filled the space inside the NICU’s suite 3M321, soon unofficially dubbed “The Schulak Suite.”
A skilled team of specialists, nurses, physician assistants, nurse practitioners, therapists and neonatology fellows kept the parents updated on the changes taking place.
In the weeks after her own discharge, Jen joined the team on their daily rounds with the triplets, writing down updated vitals and other information in a notebook. Each day brought a frustrating mix of improvement and regression.

To the Schulaks, the entire group, including the NICU nurses, respiratory, occupational and physical therapists, speech language pathologists and advanced practice clinicians, are now part of their extended family — “aunties” and “uncles” because of the months they spent providing care for the boys.
She keeps in touch with nurses and therapists from the NICU, sending them photos and videos that showcase the triplets’ blossoming personalities.
“I have such a profound respect for NICU nursing. It’s such a delicate practice,” she said.
“They know our babies inside and out, because they cared for them every minute of every day.”

For Jon Schulak, the NICU nurses helped him understand in layman’s terms the myriad challenges and changes involving the boys’ care. They also served as sounding board, reality check and pep squad as the newly minted parents of five tried to navigate the double life of raising two children at home while three more slowly improved in the hospital.
“Whatever it was that we needed, they were there, even sharing their experience of what they’ve seen over the years, The nurse practitioners and the nurses did so much more for us than I would have expected,” he said.
When it comes to caring for the complex needs of NICU patients, nurses and other staff take a whole family approach, said Lyndsay George, RN, RN-NIC, who came to know the Schulaks well over the months they spent in the NICU.
She told Schulak: “We wanted you to be able to keep your mom hat on. There are days when you are a nurse, but when you are here, you’re a mom first. You are Dylan, Trent and Nathan’s mom.”
The first five months
Watching the boys at home snuggling against their parents and chasing each other around the kitchen floor, it’s hard to imagine they were once so ill they required round-the-clock interventions.
Dylan’s parents call him a “lounge lizard” because he likes singing into microphones. Trent loves hats and scooters. Nate carries markers around by the handful.

Premature babies who miss critical weeks of development in utero can face a litany of challenges outside the womb. In addition to medical complications, they can struggle with breathing issues, digestive problems and neurodevelopmental delays. Even something as innocuous as touch can be overwhelming to a premature newborn.
To support the fragile babies’ ongoing development and improve their outcomes, caregivers from Respiratory Therapy and Pediatric Therapy joined the growing team of clinical experts overseeing the triplets’ care.
Physical therapist Dana Sutula, PT, occupational therapist Nicole Gallagher, OT, and speech-language pathologist Laura Halvorsen, SLP, focused on identifying and teaching specific techniques that would encourage each boy to achieve the development that typically happens in the final weeks of pregnancy.
The therapists also worked with the Schulaks to help them prepare for the boys’ additional needs once they were home.
“Therapeutic positioning is especially important in the beginning, so we wanted to make sure that they were well-supported to help the brain develop appropriately and also have some positive touch,” Gallagher said.
Even when the hurdles loomed large and the improvements seemed miniscule, Gallagher said, the family kept pushing on.
And it didn’t take long for the Schulak boys to find a way into her heart.
“I just love them like they’re my own little nephews,” she said.

While the Schulaks spent as much time as they could in the NICU with the boys, their other children needed them too. The couple tried to make sure that Carter, then 5, and Brynn, under 2, had some consistency despite the chaos.
Most days, Jen took Carter and Brynn to day care in the morning, then drove to the NICU where she would stay until Jon got off work and went to the hospital to relieve her. Then she picked up the other two at day care and started on their evening routine.
ChristianaCare is the only health system in Delaware named a High Performing Hospital for maternity by U.S. News & World Report.
Even two years later, Jen remains especially grateful for caregivers who made it part of their daily routine to check on the boys and treat them as if they were their own. She calls them “angels,” people like pharmacist Barbara McKinney, Pharm.D., who made a point to stop in and sit with Trent — the triplet who stayed the longest —at 3 p.m. every day when she got off work.
“Every layer of caregiver here, from Environmental Services to Pharmacy to Nutrition, went above and beyond for our family,” Schulak said.
Coming home
After spending his first three months in the NICU, Nate came home in May 2021, followed by Dylan eight days later. Trent, the most medically complex of the triplets, needed a little more time. He had a gastronomy tube (G-tube) inserted to ensure he received enough nutrition. After five months in the NICU, he joined his brothers at home.

The family of seven was finally under one roof, nearly a year after Schulak found out she was pregnant with three unexpected miracles.
The boys continued to work with caregivers from the Pediatric Therapy team as part of early intervention services through Delaware’s Child Development Watch. Improvement and development came fast.
“Those boys were trying to keep up with their older siblings,” Gallagher said.
By fall 2022, the boys were discharged from occupational and physical therapies. Two of the boys continue to receive speech services at their day care. Despite their initial struggles with eating, they are tiny chowhounds, eating and drinking with no problems. Trent is on track to have his G- tube removed in the near future.
“They’re developing and growing in a way that exceeded all expectations,” Schulak said.
“I think a lot of that has to do with the support and encouragement that we got from everyone around us. They told us to keep pushing, so the boys were able to show how extraordinary they are.”
Looking ahead
Even with an army of family, friends and other loved ones nearby – including Schulak’s Uncle Ralph, who drives Carter to school every day and helps out with the kids at home – it’s physically and emotionally draining to keep up with five young children, especially when some have complex health needs, Schulak said.

But she keeps striving for balance and looks for the positives, like the welcoming embrace of her colleagues on the PACU, where she returned to work part-time.
“Jen never, ever gets flustered. She is always on top of everything and goes with the flow no matter how critical the situation,” said colleague Lauren Speakman, RN, CCRN.
That’s a useful quality at home, Schulak said, whether it’s one brother fighting another over a book, another toddler falling in the family room or a sibling who only wants to use the purple crayon.
It’s all part of their chaos, and thanks to the dedication, caring and expertise of dozens of ChristianaCare caregivers who were there from the start, the Schulaks get to experience that every day.
For that, they feel grateful – if not perennially exhausted.
“Going through all of this has helped me have a different perspective on what it feels like for our patients,” Schulak said. “When someone can see you as a person and meets you where you are, it makes all the difference.
“When we needed something in that moment, whether it was to laugh, coffee, or step away, we had it. And that’s worth sharing.”