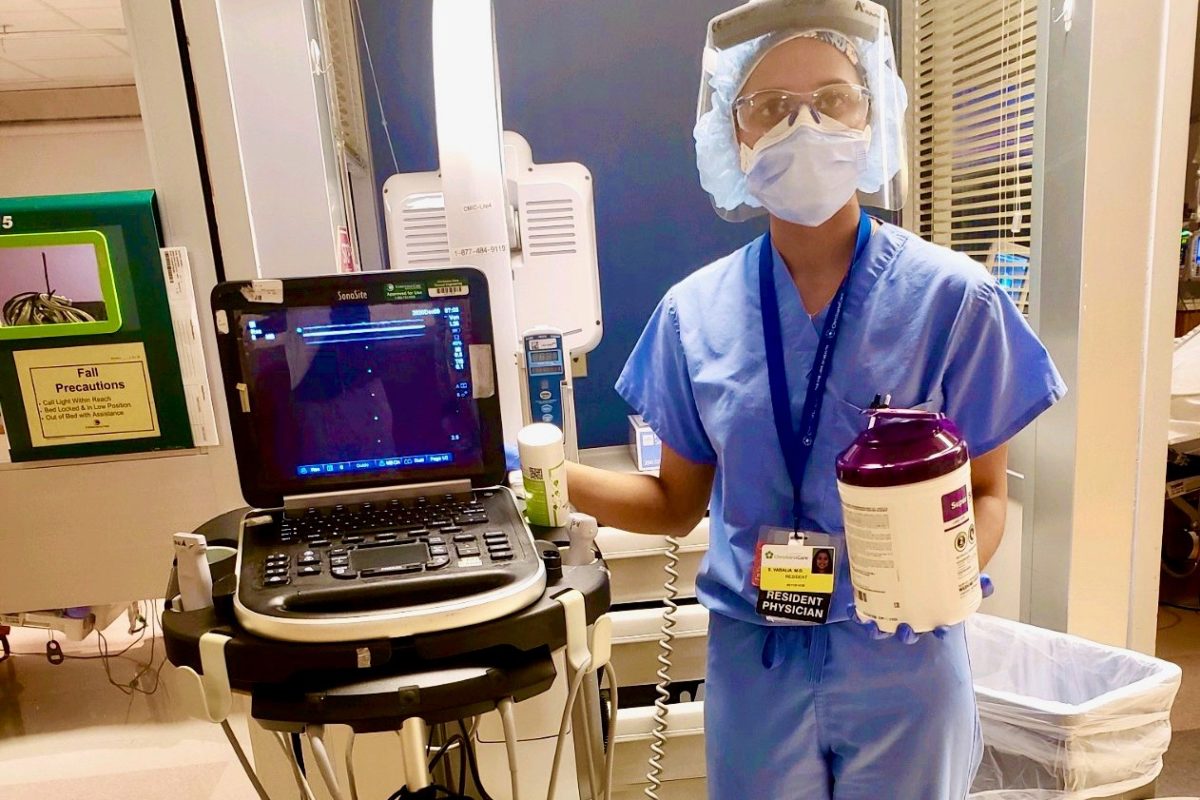
Helen Toma, M.D., MSPH, was in the midst of her residency in obstetrics and gynecology at ChristianaCare when COVID-19 cases surged in the region. To support the growing need for caregivers for these urgently ill patients, she was reassigned to the COVID-19 step-down unit.
Dr. Toma assumed she’d help with documentation duties. As it turned out, she also worked with hospitalists caring for extremely ill COVID-19 patients. An attending physician and enthusiastic educator involved her in the decision-making processes for these patients.

“While I went to the COVID-19 unit to relieve some of the stress of hospitalists who were working tirelessly to take care of patients, it ended up being a tremendous learning opportunity and period of growth for me,” she said.
Residents are medical school graduates who spend up to seven years in specialty training, depending on the program. They’re a valuable resource in a teaching hospital like ChristianaCare, which was named one of the 50 Best Teaching Hospitals for America by Washington Monthly Magazine.
The largest teaching hospital between Philadelphia and Baltimore, ChristianaCare trains 285 residents and fellows in 32 highly competitive residency and fellowship programs annually.

“We benefit from having trainees who are capable of seeing all types of patients and who can lend a hand in virtually any situation,” explained Brian Levine, M.D., associate chief academic officer in the Institute for Learning, Leadership and Development (iLEAD).
During COVID-19 spikes, the health care system mobilized residents to support the caregivers fighting to keep coronavirus cases under control. “They put their heads down and worked their tails off to take care of the patients coming to us from our community,” Dr. Levine said.
Before moving residents to different areas, ChristianaCare applied to the Accreditation Council for Graduate Medical Education (ACGME) for a pandemic emergency response exception. (The ACGME accredits residency programs.)
The exception allowed ChristianaCare to alter routine schedules and roles so residents from other specialties could support caregivers in hospital and emergency medicine. John Donnelly, M.D., FAAP, FACP, director of Medical Education in the Department of Medicine, coordinated the residents’ deployment.

Caring for the increase in patients with COVID-19 altered all residents’ schedules and conferences. However, the initiative also involved redeploying residents from a number of programs including Internal Medicine, Internal Medicine-Pediatrics, Emergency Medicine/Internal Medicine, Psychiatry, Radiology, OB/GYN, Family Medicine, Emergency and Medicine/Family Medicine.
Doctors who worked outside of their typical training did so safely and stayed within their licenses’ limits, Dr. Donnelly said.
“I anticipated that there would be an educational gain for them,” he said. “They would learn about the acute care of COVID-19 during a pandemic. In addition, they could bring expertise from their specialty areas: A psychiatry resident could weigh in on some of the psychiatric impacts of the virus, for example.”

Residents said they felt like they were part of a team. Shalini Vadalia, M.D., a combined resident in Internal Medicine and Pediatrics, valued the opportunity to support colleagues in other residency programs. The resident, who worked extra night shifts, appreciated collaborating with program and department leaders to organize the additional resident responsibilities.
“In solidarity, radiology faculty, residents and technologists supported each other to keep Imaging Services operating smoothly during resident reassignments,” said Sara Gavenonis, M.D., director of the Radiology residency program. “We are grateful to have had this opportunity to work together, adapt together and serve together.”
Learn more about ChristianaCare’s nationally acclaimed residency programs.