Each year nearly 1 million people are hospitalized for heart failure.
At its core, heart failure means the heart isn’t pumping as well as it should be, causing the body to retain unhealthy amounts of fluid. It is a complex disease that can affect patients with a number of other conditions and lead to frequent hospital stays.
To improve the health of people with heart failure, ChristianaCare has established a care standardization approach built on best practices, technology and education.
“We want to make sure patients with heart failure in our community have access to the highest-quality, guideline-based care, and care standardization is helping us achieve this,” said Kelly Whitmarsh, MS, MBS, administrative director of the cardiovascular program.
In care standardization, doctors, nurses and other care providers work across specialties and care settings to implement standardized but individualized plans of care informed by the most up-to-date information.
Heart failure experts frequently meet with caregivers from other specialties such as nutrition, social work, pharmacy and behavioral health to discuss the best care for heart failure patients.

“We reach across specialties and services to optimize care,” said Kirk Garratt, M.D., MSc, medical director of the Center for Heart & Vascular Health.
The work helps ensure that patients consistently receive the best coordinate care for their individual needs at every touchpoint with ChristianaCare.
It’s working, said Sourin Banerji, M.D., medical director of the advanced heart failure mechanical circulatory support program.
ChristianaCare’s 30-day heart failure readmission rate is 17.5% — below the national average of 25%.
“We’re seeing mortality rates fall. We’re seeing the need for hospital readmission fall. We’re seeing compliance with guideline directed medical therapy increase,” Dr. Garratt said. “These are all things we’re hoping to gain, and we see the fruits of that effort now.”
To better treat heart failure, caregivers at the Center for Heart & Vascular Health partnered with caregivers in the Center for Strategic Information Management to develop a machine-learning algorithm that can predict a hospitalized patient’s risk for heart failure.
“Heart failure can take time to diagnose,” said Whitmarsh. “Now the prediction score allows us to identify patients more quickly than ever before. It helps us begin guideline-based treatments and disease education more efficiently.”
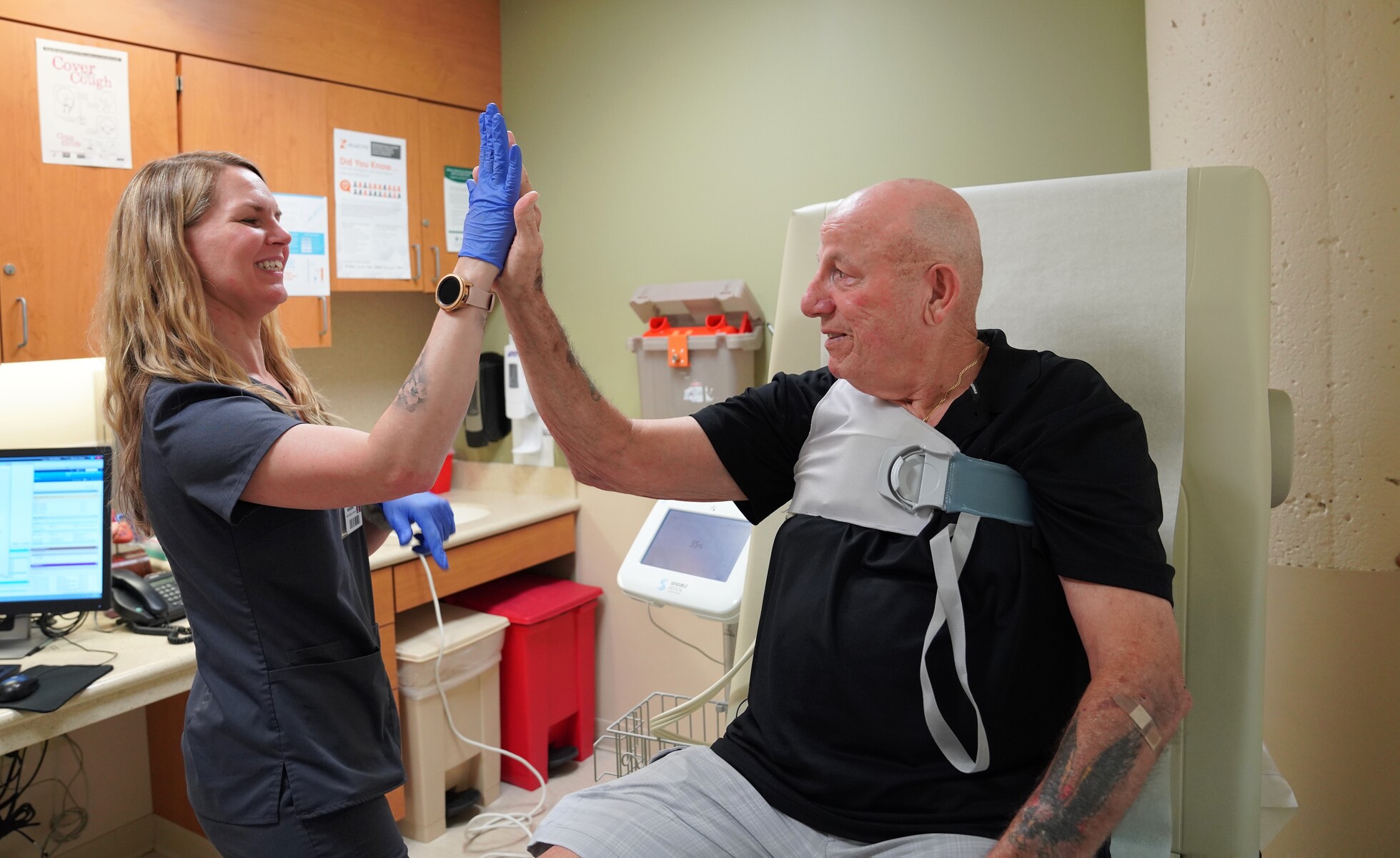
A bridge to better health
Technological advances continue to support patients throughout their hospital stay and after discharge. Patients now have the opportunity to attend a four-week program at the Heart Failure Bridge Clinic at Christiana Hospital. The Bridge Clinic is a special care unit constructed specifically to assure the highest risk patients get what’s referred to as outpatient intensive care for their heart failure.
During their time in the clinic, they continue treatments they experienced in the hospital while they begin a program of monitoring that enables the care team to identify emerging problems and intervene as needed. The monitoring program uses a wearable technology called the ReDS™ vest. ReDS stands for “remote dielectric sensing.”

“Heart failure has a high rate of readmission within 30 days after discharge – largely due to fluid build-up. We use the ReDS vest to detect early fluid accumulation in the patient’s lungs, which can occur before they feel any signs or symptoms of worsening heart failure,” Whitmarsh said.
“Now we can treat patients with early fluid accumulation to prevent emergency room visits and hospital admissions.”
ReDS vest measurements can also be taken for patients in their homes if transportation is a barrier. Home health aides from ChristianaCare’s Visiting Nurse Association take the reading in patients’ homes, and nurse care coordinators monitor the measurements and coordinate interventions with the patient’s primary medical team.
The multi-disciplinary approach to care also continues in the outpatient setting.
While at the Heart Failure Bridge Clinic, patients continue to have access to supportive and palliative care and behavioral health services.
Caregivers also work closely with primary care providers, cardiologists and home health care providers to ensure patients are receiving the same standard of care after discharge.
“We involve the patient’s caregivers in the Bridge Clinic visits as much as possible,” said Whitmarsh. “Heart failure is a challenging condition, and patients and their caregivers need support.”
Focused on education
Complementing the technology is patient education, making patients and caregivers true partners in their care.
“There is great value in education about the signs and symptoms of worsening heart failure so patients can alert their clinicians and their caregivers,” Dr. Banerji said.
“We also educate patients on how to monitor their weight, their sodium restriction and fluid restriction. These are very common touch points of heart failure hospitalizations.”
Through care standardization measures, heart failure physicians say they are moving the needle on both quality metrics and cost metrics.
“Most satisfying is that we see clearly how much patients value the education and partnership to help them live their best lives,” Dr. Banerji said.
Learn more about ChristianaCare’s Heart Failure Program.