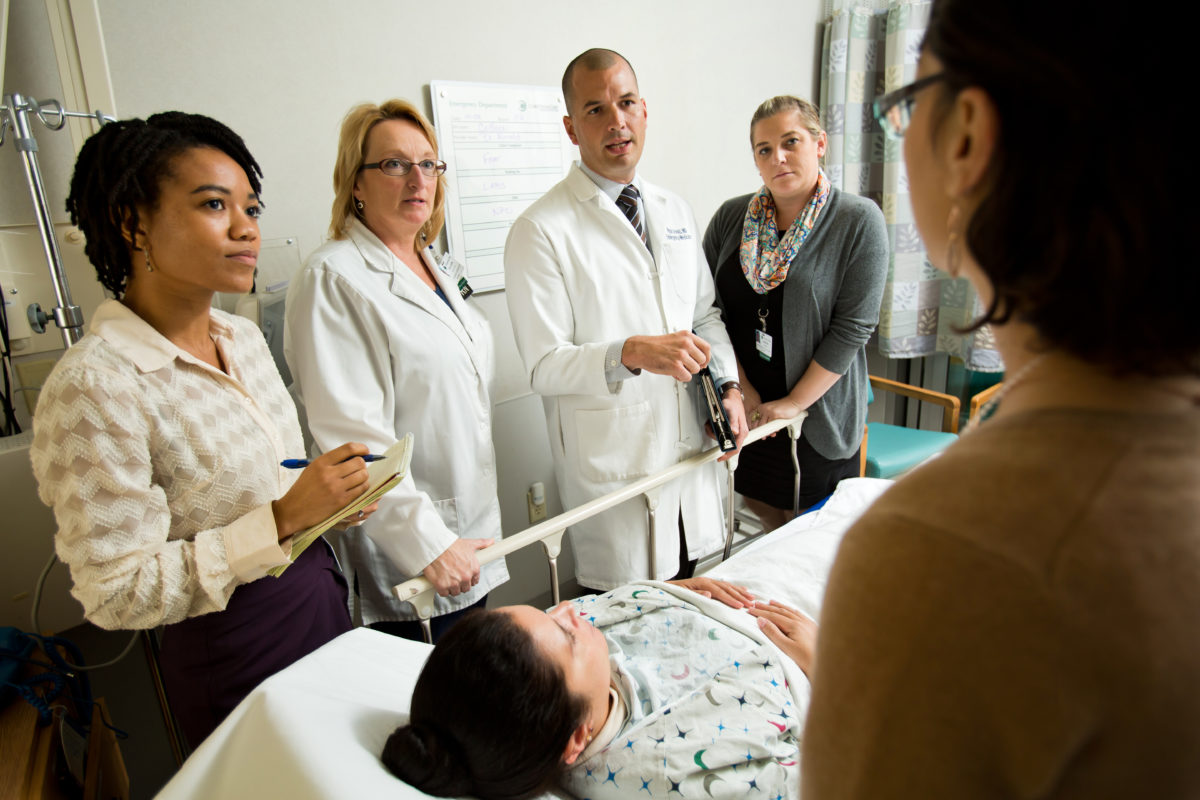
Sepsis, a life-threatening organ dysfunction, causes nearly half of all U.S. hospital deaths, accruing $20 billion in treatment costs each year.
Now, a team from the Value Institute at Christiana Care Health System is determined to change that landscape. It is pioneering an innovative approach to detect and treat sepsis, which infects about 1 million people annually, killing a quarter of them.
Their research project, “Signaling Sepsis: Developing a Framework to Optimize Alert Design,” recently won a highly competitive, four-year grant from the U.S. National Library of Medicine funded through the U.S. National Institutes of Health. The study is a collaboration with the University of Pennsylvania, the University of Michigan and the Medical University of South Carolina.
“Our research has the potential to evolve the electronic medical record system and significantly impact the design of clinical care and practice,” the team wrote in its application for the R01 Research Project Grant, the original and historically oldest grant mechanism of the U.S. National Institutes of Health. “This research will advance what is known in the field and has the capacity to improve medical case decision-making, delivery, and health of patients and of the public.”

It is the first such grant at this level to originate with Christiana Care as the leading research entity, said the project’s lead investigator, Kristen Miller, DrPH, MSPH and the Value Institute’s associate director of Human Factors.
The project is unique on several fronts. First, it focuses on providers in medical and surgical units, not those in an emergency setting where workers are more used to looking for deadly vital signs.
“National data show a higher mortality rate for inpatients that develop severe sepsis or septic shock on a medical or surgical unit compared to those that present to the emergency department and are admitted directly to the Intensive Care Unit,” said Eric V. Jackson Jr., M.D., MBA, director of the Value Institute’s Center for Health Care Delivery Science and associate director of the Value Institute.

“Clinicians and nurses on the general medical-surgical units are not as oriented or experienced in recognizing and diagnosing septic patients,” he said. “Selecting these units provides enormous potential to save and improve lives, understanding that these patients would benefit the most from a predictive tool to drive action for decompensating patients,” Dr. Jackson said.
Sepsis occurs when a body is experiencing a severe response to bacterial, fungal, viral or yeast infection. The release of chemicals into the bloodstream to fight the infection causes widespread inflammation that eventually can slow blood flow and damage organs. In the later stages, sepsis can progress to life-threatening organ failure and shock.
The tricky part is that sepsis often hides behind other diagnoses, escaping detection. It can attack any organ in people of any age, and it does: roughly one in every 23 patients admitted to the hospital will develop a sepsis infection.

“It’s not as clear-cut as, say, a heart attack,” said Vinay Maheshwari, M.D., MHCDS, FCCP, vice chair of Medicine and associate physician operations leader for the Acute Medicine Service Line. “Sepsis has such a broad presentation. It can creep up on providers, who don’t necessarily connect the dots.”
Early and accurate identification of sepsis is critical to survival. For every hour that treatment is delayed, the chance of dying from sepsis increases 7.5 percent.
The signs can be subtle, which is where the computer-assisted guidance comes in. Instead of having to hunt among patients’ medical records to piece together the big picture, the alert system will assess danger by recording such data as abnormalities in vital signs, respiratory rate, kidney and other organ function and mental status.
“It’s important to have a tool specific to this disease so treatment is appropriate and accurate, and providers are using it consistently,” said Ryan Arnold, M.D., MA, research director in the Department of Emergency Medicine, clinical investigator at the Value Institute and co-primary investigator on the project.
In another unique twist, the research won’t be studying patients per se, but their providers. That is, the team will test various ways to display information that will most effectively alert the providers of possible danger and guide them through evidence-based best practices to turn the infection around before it becomes deadly.
The key to success is in having a strong understanding of human behavior, which is Miller’s specialty, as she has studied public health, cognitive psychology and industrial engineering.
“One of my research interests is the design, implementation and evaluation of clinical bioinformatics electronic decision support — how you display information in a meaningful way,” she said. “Research addressing the changing nature of clinical decision support systems is different from what you usually see.”
Part of the 4-year, $1.4 million grant is $40,000 for a mobile usability lab. Researchers will use the lab to collaborate with providers in rural, urban, academic and community settings.
“Our objective is to determine the best way to provide a sepsis alert to improve decision-making in the dynamic, fragmented health care work environment,” Miller said. “We hypothesize that the design of the alert plays a significant role in provider recognition and response. Ultimately, it will improve the response of providers and result in better, quicker and most appropriate treatments.”
Dr. Maheshwari is intrigued with the approach.
“In today’s digital world, we get inundated with alerts and flags, and after a time they just become noise,” he said. “The exciting thing about this is we have folks like Kristen who can tell you what makes a person act one way or another — do they respond to green or red?
“This project is about taking the information that we have in our computer system and presenting it to providers in a way that they are made aware that sepsis is present. Then, they are guided to make the right treatment choices.”
The project is part of a growing national campaign to bring awareness to this deadly disease. Sepsis received national attention after physicians in the emergency department of a New York hospital in 2012 discharged a 12-year-old boy who had cut his arm diving for a basketball at school. Three days later, Rory Staunton died of sepsis in the ICU.
“One of the things that’s so tragic is sepsis can occur at any age,” Dr. Arnold said. “While it is more prevalent in the elderly, whose immune systems are declining, or the very young, whose immune systems are developing, we still have 20-, 30-, 40-year-olds dying solely from that infection.”
Dr. Arnold said the awareness campaign launched by Rory’s family shined an appropriate light on the condition.
“It was a landmark change in defining the at-risk population. The message was: Sepsis can develop from any infection, in any population, and needs vigilant screening” he said.
“This is a disease I’ve focused on for the past 12 years, but we always called it the ‘orphan disease’ because it wasn’t focused on,” he said. “It’s exciting to have the opportunity to set the standard and be an industry leader in this disease process. Christiana Care is on the map now, leading the way.”