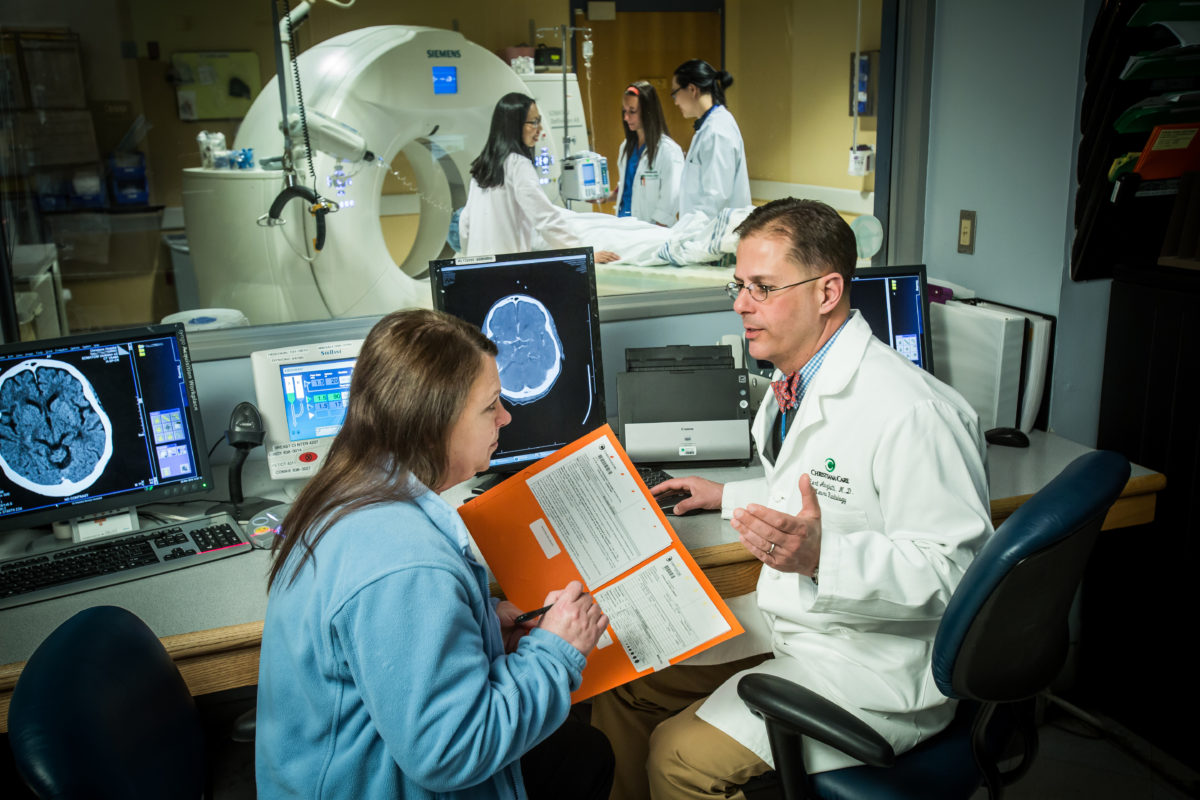
With a landmark Joint Commission certification and top marks from the American Heart Association (AHA), Christiana Care Health System is earning national recognition in stroke care.
These honors, though, are but a reflection of the way patients and their families measure Christiana Care’s dedication to stroke care: in lives saved and disability averted. No matter your criterion, the conclusion is the same. Christiana Care has attained the highest echelon of stroke care.
By methodically deconstructing the myriad processes involved in treating ischemic stroke, Christiana Care’s stroke team has stripped out non-essential steps. This laser focus has allowed Christiana Care to shave precious minutes off the time before stroke treatment is administered, an accomplishment that saves lives and reduces the long-term disability for hundreds of patients who seek treatment here.
Moreover, this focus enabled Christiana Hospital to exceed the guidelines set forth by the American Health Association in the swift treatment of ischemic stroke, which accounts for 87 percent of all strokes. This form of stroke involves an obstruction of a blood vessel supplying oxygen to the brain and is differentiated from a hemorrhagic stroke, wherein a blood vessel ruptures in the brain. Together, both forms of stroke translate into the country’s fifth leading cause of death and its leading cause of preventable disability.
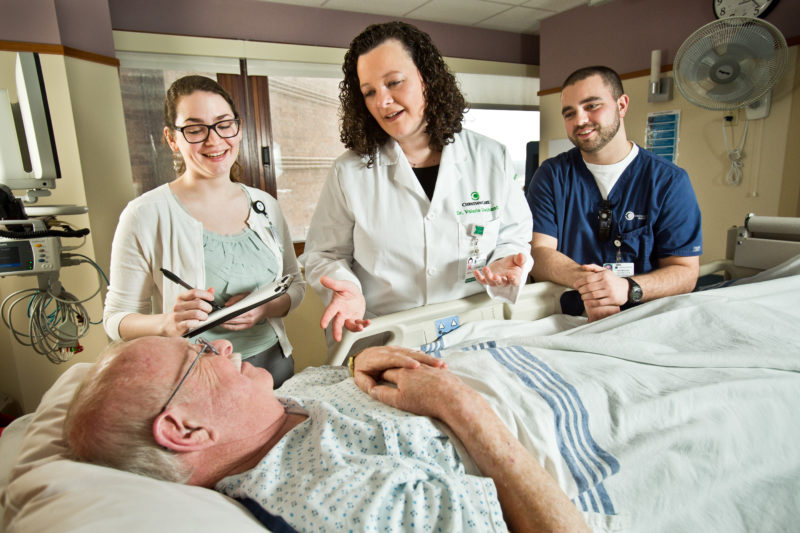
Christiana Care treats almost 2,000 strokes a year, putting it in the top 10 nationwide in patient volume.
Jonathan Raser-Schramm, M.D., Ph.D., medical director of the Christiana Care Stroke Program, credits this success to “an amazing team that works together to provide excellent care to our stroke patients.”
The next major goal is to collaborate with physicians and hospitals across the state to improve stroke care for all Delawareans — whether or not the patient is served by Christiana Care.
Saving lives by saving time
A key Christiana Care objective in recent years has been the reduction of the time that elapses between entry to the emergency department and administration of a clot-dissolving drug called tissue plasminogen activator, or tPA — referred to as “door-to-needle time.” The national target is an average of 45 minutes. Christiana Care has whittled the time down to 35 minutes on average.
Because stroke treatment is about saving brain cells, which don’t regenerate once they die, fast treatment is crucial. During a major stroke, 1.9 million neurons die every minute. In addition, for every 15 minutes faster tPA is administered, there is a 4 percent decrease in mortality prior to discharge and 4 percent greater odds of walking independently at discharge.
Though fast administration of tPA is elemental in stroke care, a CT scan is required before it can be used. That’s partly because the drug cannot be administered in someone with a hemorrhagic stroke. And if too much time has elapsed, there may not be enough healthy brain tissue near the stroke to salvage, so effective use of tPA is limited to four and a half hours after symptom onset.
Break apart acute ischemic stroke care into its constituent processes and you’ll find scores of individual staff performing their tasks, each with a time cost, said Kert Anzilotti, M.D., MBA, physician leader in the Neurosciences Service Line and chair of Radiology. A workflow analysis by Christiana Care revealed tasks that could be safely performed later, after the acute phase of treatment was over. For example, detailed Emergency Department registration didn’t need to be done at admission. When brain cells are dying with each passing second, the paperwork could wait. And behind essential tasks were ways to save time. Simply moving the IV kit out of a storage area beforehand saves a minute.
These iterative improvements and many others have dropped the average door-to-needle time at Christiana Hospital from about 90 minutes in 2012 to about 35 minutes today.
How a patient experiences care
What does a stroke look like from the patient’s perspective? Imagine the case of a Newark woman whose husband calls 911 after noticing his wife can’t speak clearly and has weakness in one arm. (Other stroke symptoms include confusion, loss of balance, one-sided numbness, visual changes and facial drooping.)
First, the emergency responders, suspecting a stroke, conduct more screening questions and ascertain what medications the patient is taking. En route to the Emergency Department, the responders call Christiana Hospital on a special medic line and report the patient’s symptoms. Together, the team decides to call a prehospital stroke alert, which includes the patient’s estimated time of arrival at the hospital.
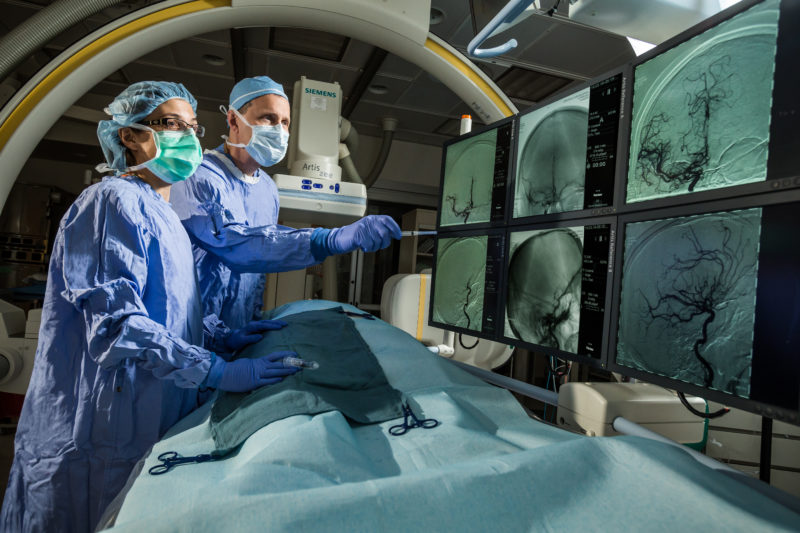
At the hospital, this alert triggers an overhead announcement and a page to the stroke team, and informs radiology technologists to free up a CT scanner.
When the patient arrives, she is evaluated to ensure she’s stable enough to proceed to imaging. A limited number of tests are performed at this point, including a neurological examination to help determine the severity of the stroke.
Next, a non-contrast head CT and a CT angiogram of the head and neck are obtained.
A neuroradiologist interprets dozens of images as they first appear on the screen. The analysis finds no intracranial bleeding, and intravenous tPA administration begins immediately, while the patient is still on the CT scanner table.
Meanwhile, a parallel investigation is determining whether mechanical thrombectomy is appropriate. In this case, the team decides to go forward with the procedure, and a stent is threaded into the affected intracranial artery. As the stent reaches the clot, it expands and becomes enmeshed with the clot so that when the stent is removed, the clot also is removed.
The patient is then taken to the Lanny Edelsohn, M.D., Neuro Critical Care Unit at Christiana Hospital, where she is closely monitored and discharged the next day. Her treatment has spared her the life-altering consequences so often seen in major strokes. She receives a personalized evaluation resulting in medication, lifestyle and rehabilitative therapy recommendations. She will return to the Stroke Clinic for longitudinal care by a stroke specialist.
Journey to the top
Mary Ciechanowski, MSN, APRN, ACNS- BC, CCRN, is an advanced practice nurse with Christiana Care’s stroke program who has worked in neurosciences for 28 years. She said the last decade has brought steady improvements in stroke care. One of the team’s guiding principles is to think about patients as if they were members of their own family.
“We all feel if we or our families were the patients, we would want the best care possible,” Ciechanowski said.
In 2006, the formation of a stroke unit began the process of enabling nurses and physicians to become experts in stroke care. Another focus at that time was increasing the use of tPA, which is still the AHA’s gold standard for treating ischemic stroke.
In 2007, Christiana Care hired its first neurointerventionalist, Barbara Albani, M.D., now Neurointerventional Surgery medical director. Neurointerventional procedures expanded urgent stroke treatment options for the Delaware community.
Meanwhile, Christiana Care noticed a gap in comprehensive stroke centers in the region: there were such facilities in Philadelphia and Baltimore but none in Delaware. After about two years of preparation for reviewers from the Joint Commission, Christiana Hospital achieved certification as a comprehensive stroke center in 2014. It was recertified this year. This comprehensive designation allows Christiana Care to participate in medical studies and offer the newest diagnostic and treatment options to patients. Clinical trials are now under way to evaluate the use of tPA in mild strokes and evaluate endovascular therapy more than six hours after the onset of symptoms.
This year, Christiana Hospital received a pair of recognitions from the American Heart Association: the Get With the Guidelines Stroke Gold Plus Quality Award and the Target: Stroke Honor Roll Elite Plus. Both are tiered awards. Get With the Guidelines has four levels and Target: Stroke has three. Christiana Care received the highest designation in each case.
Get With the Guidelines Stroke recognized Christiana Care for adherence to a set of best practices in stroke care, and Target: Stroke was largely a recognition of reductions in door-to-needle times. Wilmington Hospital was first certified as a primary stroke center in 2009 and has been recertified biannually since. This designation, one level below comprehensive, means the hospital has met Joint Commission standards in 14 areas, including treatment capabilities, staff education and performance measures.
In raising standards at Wilmington Hospital, specialists at Christiana Hospital have been using video conferencing with emergency medicine physicians to help make diagnoses and find the right treatment. Their tools? An iPad secured to an IV pole.
“I love the low-cost, gritty solution,” Dr. Anzilotti said. “They’re not there, but it’s like they’re there.”
Douglas Huisenga, MPT, ATC, manager of the Neurosciences Program, said any one of these awards or certifications would have been noteworthy by itself. The fact that Christiana Care fit all of these accomplishments into one year is a striking validation of their work, he said.
Dr. Raser-Schramm, the stroke program’s medical director, said the central requirement for certification as a Comprehensive Stroke Center is “that dedication to continuous improvement in care.”

Empowered nurses
Kaci Rainey, MSN, RN, CEN, an Emergency Department nurse for nine years, had an idea about how to save time in stroke care. As a trauma nurse, Rainey recalls a CT technician receiving verbal orders from a physician for CT imaging during the trauma alert process. But the stroke process required an Emergency Department physician to put an order in, which could cause delays, so she suggested moving to verbal orders for CT imaging for stroke patients.
Rainey gives much of the credit to Ciechanowski, the advanced practice nurse. “Her willingness to listen to what I had to say was transformative,” Rainey said. “Ideas can’t go anywhere without someone to listen.”
Rainey had still more ideas, including one about how to treat stroke patients once they’ve reentered the Emergency Department after they’ve entered their initial treatment (with tPA, for example). These patients require neurological testing every 15 minutes, which makes it difficult for nurses to give other patients the attention they deserve. Furthermore, her literature review found that moving patients more quickly out of the Emergency Department has been associated with decreased mortality.
In collaboration with other team members, Rainey helped develop a process whereby a nurse in the Neuro Critical Care Unit is automatically notified after a stroke treatment is administered. If a bed is available, the critical care unit nurse comes to the Emergency Department. These critical care nurses have also picked up the skills to transport patients, freeing up yet more time for ED nurses.
This process, implemented in August 2014, has resulted in a 78 percent decrease to stroke patients’ length of stay in the Emergency Department.
Her work off the floor is made possible by Christiana Care’s decision to allow nurses time off their regular duties to work on projects.
“They show us they value nurses,” Rainey said.
A strong chain
As a way to recognize employees who recognize stroke, Dr. Albani awards clock-shaped pins — a nod to stroke’s time-sensitive treatment — to employees who notice a patient’s stroke symptoms.
“Stroke work is a team sport,” she said. “You need every link to be strong.”
Christiana Care’s stroke program is made up of dozens of such links, each working to serve neighbors with swift effective treatment that helps stroke victims return to health and normalcy.