Patient praises her Cyberknife treatment experience


In August 2009, Myrle Bowe, a patient at the Helen F. Graham Cancer Center, elected to have CyberKnife robotic radiosurgery to treat a brain tumor. This is her account:
My robust life as a senior citizen included volunteering, visiting grandchildren, pursuing a second career and having fun—until a tumor appeared.
For years, I had and ignored regular headaches. Then in late 2008, I mentioned a new, sharper headache to my primary-care physician. He immediately referred me to neurosurgeon Kennedy Yalamanchili, M.D., of the Delaware Neurosurgical Group
CT and MRI scans revealed a lump—a meningioma tumor the size of my grandson’s Matchbox car. The good news was that this type of tumor grows slowly and was very unlikely to be cancerous. It was positioned at the front of my head on the left side, on the covering of the brain. It was neither invading the brain nor pressing on anything that would interfere with vital functions like vision, hearing or the pituitary gland.
It was unclear whether the tumor was causing the occasional sharp head pain I felt. I am rarely without a headache; they just varied in intensity. The new headaches added to my usual sinus, allergy, tension and migraine problems. I only used over-the-counter pain medications to get relief.
From discussions with Dr. Yalamanchili and Internet research, I learned there are three treatment options, unless there’s a drastic change:
Wait and see—put up with sharp headaches plus my usual migraines and do an MRI in a year.
Have CyberKnife radiation now or later to destroy the tissue—but not know whether the tumor is cancerous.
Have conventional surgery and test for cancer, maybe followed by antiseizure drugs, chemo and aftereffects.
What to do? My initial decision was wait and see and ignore it as long as possible (stick my head in the sand). I had not said much about it, even to family. I knew their concern would come down to seizures. Since my work involved a considerable amount of driving in Delaware and adjacent states, seizures were a major concern.
The first option was not feasible. I had to do something. Since my previous experiences with anesthesia (delivering two babies) were not pleasant, surgery on my skull did not appeal to me.
I dithered for three months but eventually concluded that Cyberknife was my best treatment option. I could have had radiation in Philadelphia or Baltimore at any one of several treatment centers, but the more I learned about the Helen F. Graham Cancer Center and Cyberknife, the more I was reassured that this was the right choice.
From my first meeting with Karen Karchner, the CyberKnife care coordinator at the Helen F. Graham Cancer Center, through the succession of appointments with radiologist Sunjay Shah, M.D., and appointments with radiation therapists and other staff, the attitude of every person I met at the cancer center communicated that in addition to providing state-of-the-science treatment, my comfort and well-being were important. Wait-time was always short, explanations about procedures clear, and my questions were treated with respect and a desire to have me understand the process.
Following a consultation with Dr. Shah, the next appointment was for shaping a mesh mask—called an Aquaplast—to the contours of my face. (Think fencing mask, except larger mesh.) The fabric felt like a warm washcloth and stayed on until it dried and set. During treatment the mask would be clipped to the head frame on the treatment table to hold my head still.
After the necessary lab tests and another MRI, the CyberKnife procedure was scheduled for half-hour treatments on three consecutive mornings in mid-August 2009. Meanwhile, the neurosurgeon and Dr. Shah precisely mapped, or contoured, the tumor so that therapists could direct radiation to it alone.
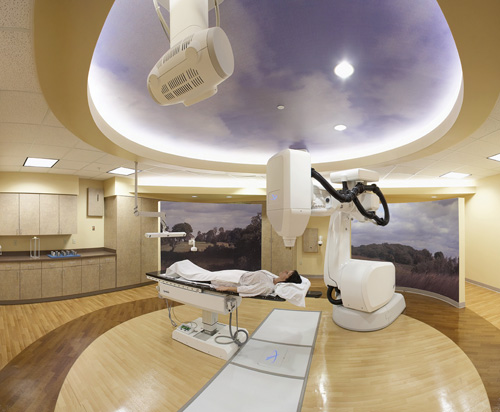
For the treatment I was lying on a padded table with a light blanket over me and a safety belt fastened. The face mask neither interfered with watching beautiful scenes on a ceiling TV nor listening to the accompanying relaxing music.
From the next room, the radiation therapists guided a space-age equipment arm to different positions around my head. If I had difficulty or discomfort with anything, I was assured that I only had to ask and they would stop to take care of it. There was no problem, no stress. Relaxation techniques I had learned put me into a dreamlike state.
My daughter had taken me to the cancer center the day of the first treatment, in case I did not feel like driving home. As it turned out, I had no ill effects at all. After that I drove myself to and from the cancer center.
Four months later, in December 2009, I had a follow-up MRI and an appointment with Dr. Shah. The good news was that the tumor had stopped growing. It is expected to shrink over time, but the smaller version will remain and will show on an MRI. Barring unforeseen events, I am to have an MRI in December 2010 and probably each year thereafter. No long-term effects are expected from the radiation.
I am extremely grateful to everyone at the Graham Center who helped me. I know there are many patients with more serious conditions than I had, and everyone I have talked to feel that there is no better source of treatment. We are fortunate to have it in Delaware.