Delaware’s First Cohort of Doctoral Nurse Anesthesiology Students Begins Training at ChristianaCare
ChristianaCare plays a leading role in a partnership building a homegrown pipeline for Delaware’s operating rooms
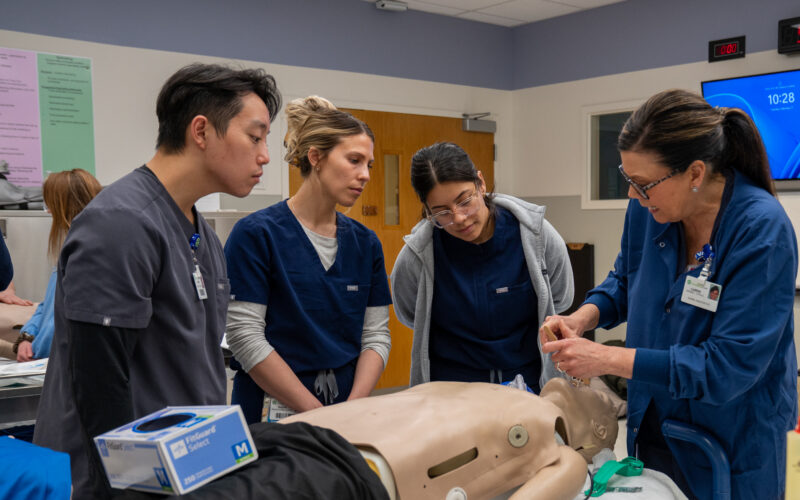
Inside ChristianaCare’s simulation lab, an instructor coached Sarah Sorowice, BSN, RN, on threading a flexible scope toward a manikin’s airway — carefully, deliberately, reading every cue. Six weeks of lectures, anatomy and pharmacology classes had been building to this first day of interactive, hands-on training.
“Getting reminded about why we’re doing this and what the ultimate goal is,” Sorowice said, “has been really encouraging.”
Sorowice came to the program from ChristianaCare’s Neuro Critical Care Unit. She loved the intensity of critical care yet found herself drawn to a role with a sharper focus on patient comfort. Working part-time alongside an anesthesia team had shown her the path. Now, she is one of 25 students in the inaugural class of the Delaware Nurse Anesthesiology Program — the state’s first doctoral program of its kind.
The program’s first cohort includes nine ChristianaCare nurses alongside experienced critical care nurses from other regional health systems.
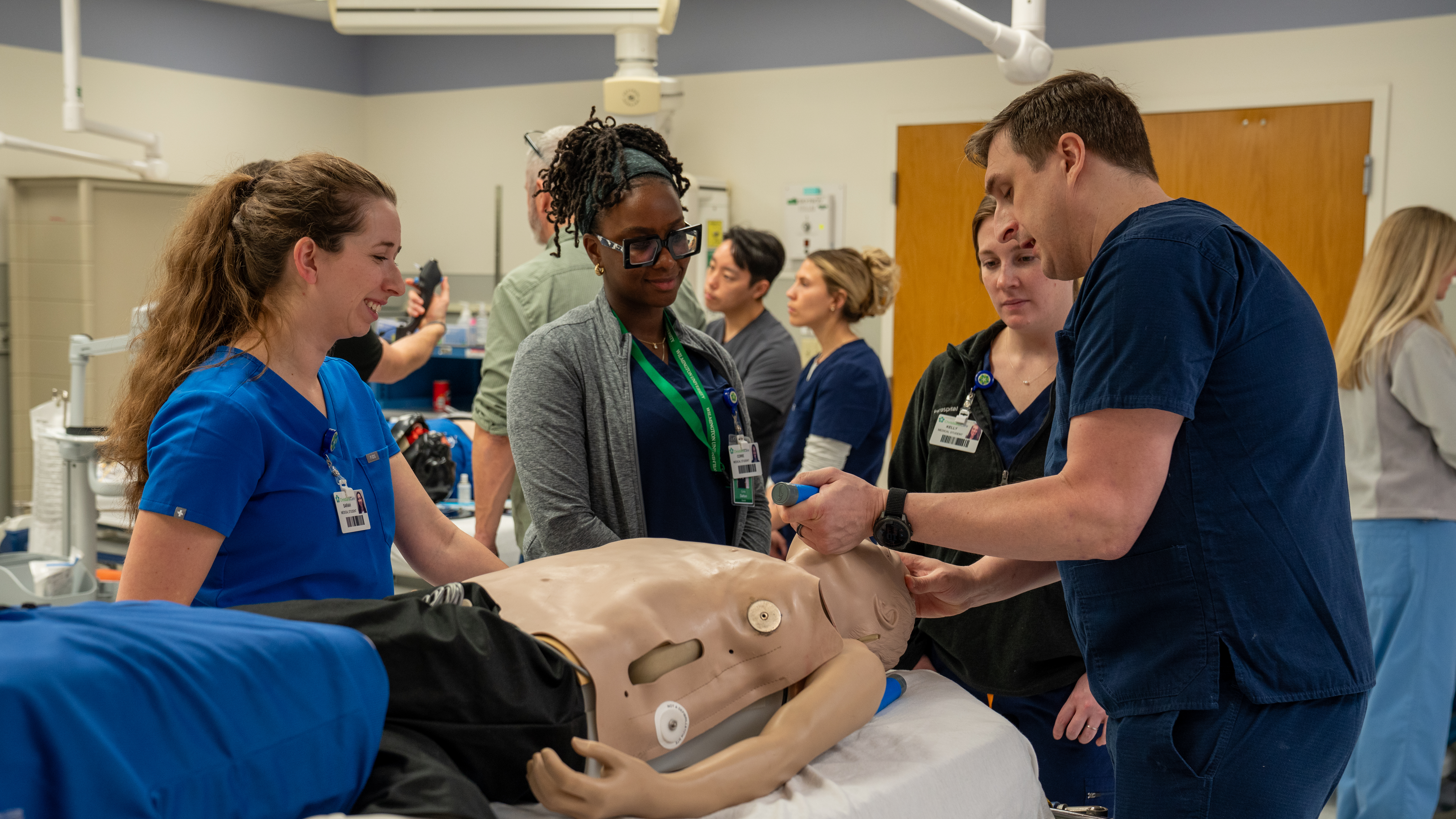
Prior to this year, a Delaware nurse who wanted to become a Certified Registered Nurse Anesthetist (CRNA) had to leave the state to train. Now nurses like Sorowice get to grow at home.
The nurse anesthesiology program was announced in October 2024 and launched in January 2026 as a partnership of ChristianaCare and Wilmington University with the support of Anesthesia Services, P.A. (ASPA), the largest anesthesia group in Delaware. The full-time, 36-month program leads to a Doctor of Nursing Practice degree and prepares graduates to sit for the national certification exam (NCE). Students are expected to log at least 2,500 clinical hours before graduating.
Growing Local Talent to Fill a Critical Need
Delaware has a strong pool of critical care nurses and a growing demand for anesthesia professionals. The U.S. Bureau of Labor Statistics projects 38% growth in nurse anesthetist employment by 2032, and many of Delaware’s experienced CRNAs are nearing retirement. ChristianaCare has long served as a clinical training site for nurse anesthesia students enrolled in Pennsylvania programs, but without a Delaware-based degree program, many of those nurses ended up staying where they studied.
ASPA saw an opening and approached ChristianaCare about building a program here. The response was immediate: the first cycle drew 250 applicants. When the portal opened January 20 for the next cohort, beginning in January 2027 and approved for up to 35 students, nearly 200 applications arrived within weeks. Applications will be accepted through April 30.
Interested in a career as a nurse anesthetist? Learn more here.
Jacqueline Mainwaring, PhD, DNP, CRNA, trained as a nurse anesthetist at ChristianaCare in the 1990s, then spent years as faculty and eventually director of the nurse anesthesia program at Thomas Jefferson University before returning to Delaware to build this one. She is the program’s inaugural director and an associate professor at Wilmington University.
“Many of our graduates will stay and practice in the same communities where they trained. That continuity of care and commitment to community matters.”

A Program Built on Longtime Experience
Among the subject matter experts working with this first cohort is Cathy Loughead, MS, CRNA, who has been at ChristianaCare for nearly 40 years. Two years ahead of Mainwaring in her own training, she precepted her in the operating room. Now she is watching the students Mainwaring recruited rotate through the same fundamentals.
For Loughead, the simulation lab represents a meaningful improvement over how her own generation was trained. In her program, students completed several weeks of didactic coursework and then went directly into clinical settings. She relishes the opportunity to help students learn to apply their critical thinking skills.
“This is a great job — it’s all thinking work, all day long,” she said. “We’re there for patient safety. That patient is completely in your hands, and your whole focus is getting them through safely and waking up well.”
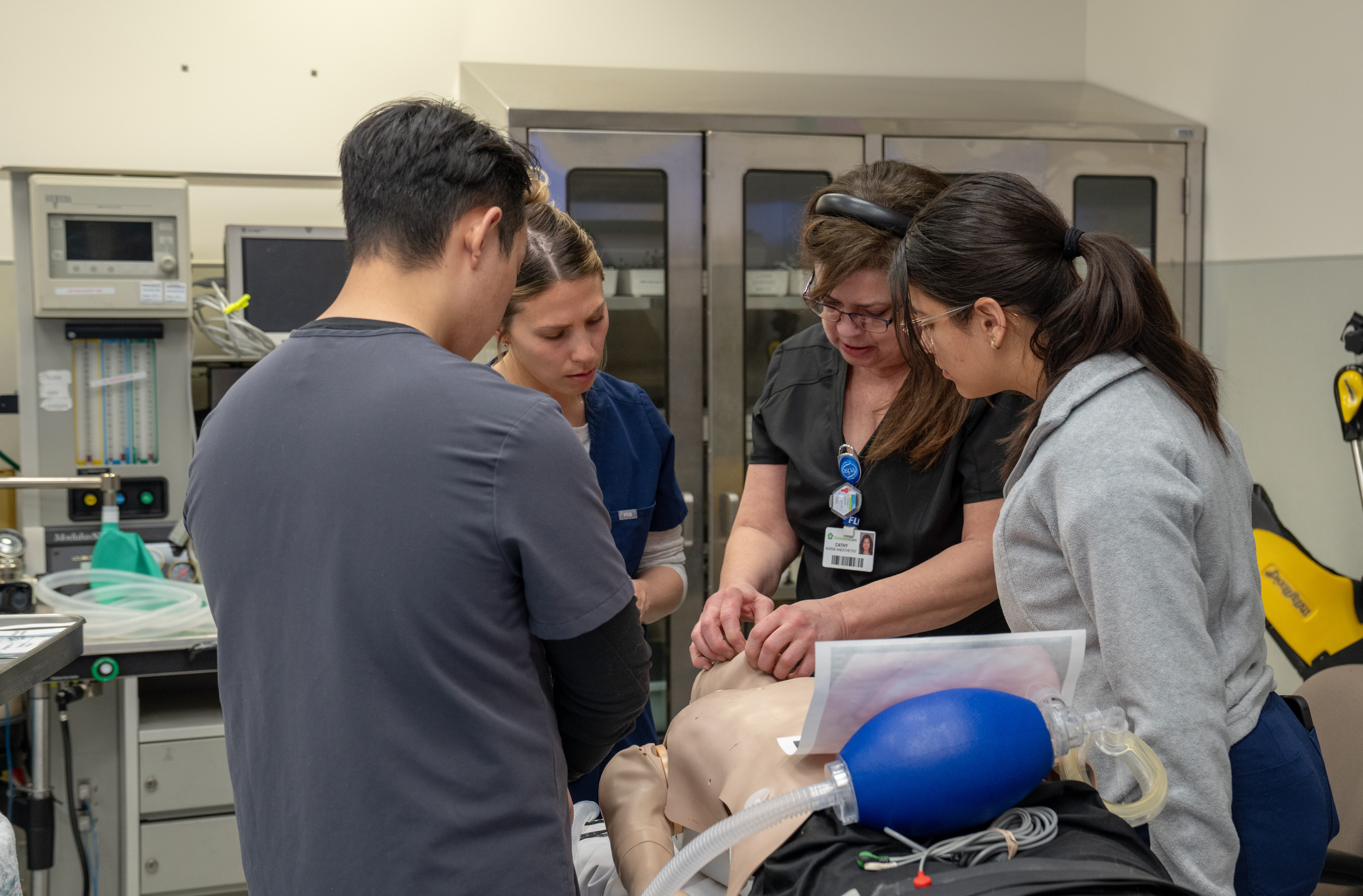
The program also places strong emphasis on experiential learning. Under the leadership of Kristen Simmons, DNP, CRNA, CHSE, assistant director and a certified healthcare simulation educator, students engage in simulation and skills labs early and often. In the simulation lab, Simmons guides students through deliberate, hands-on practice in a psychologically safe environment, allowing them to build technical skills, clinical judgment, and confidence before entering the clinical setting.
Inside ChristianaCare’s Innovative Training Center
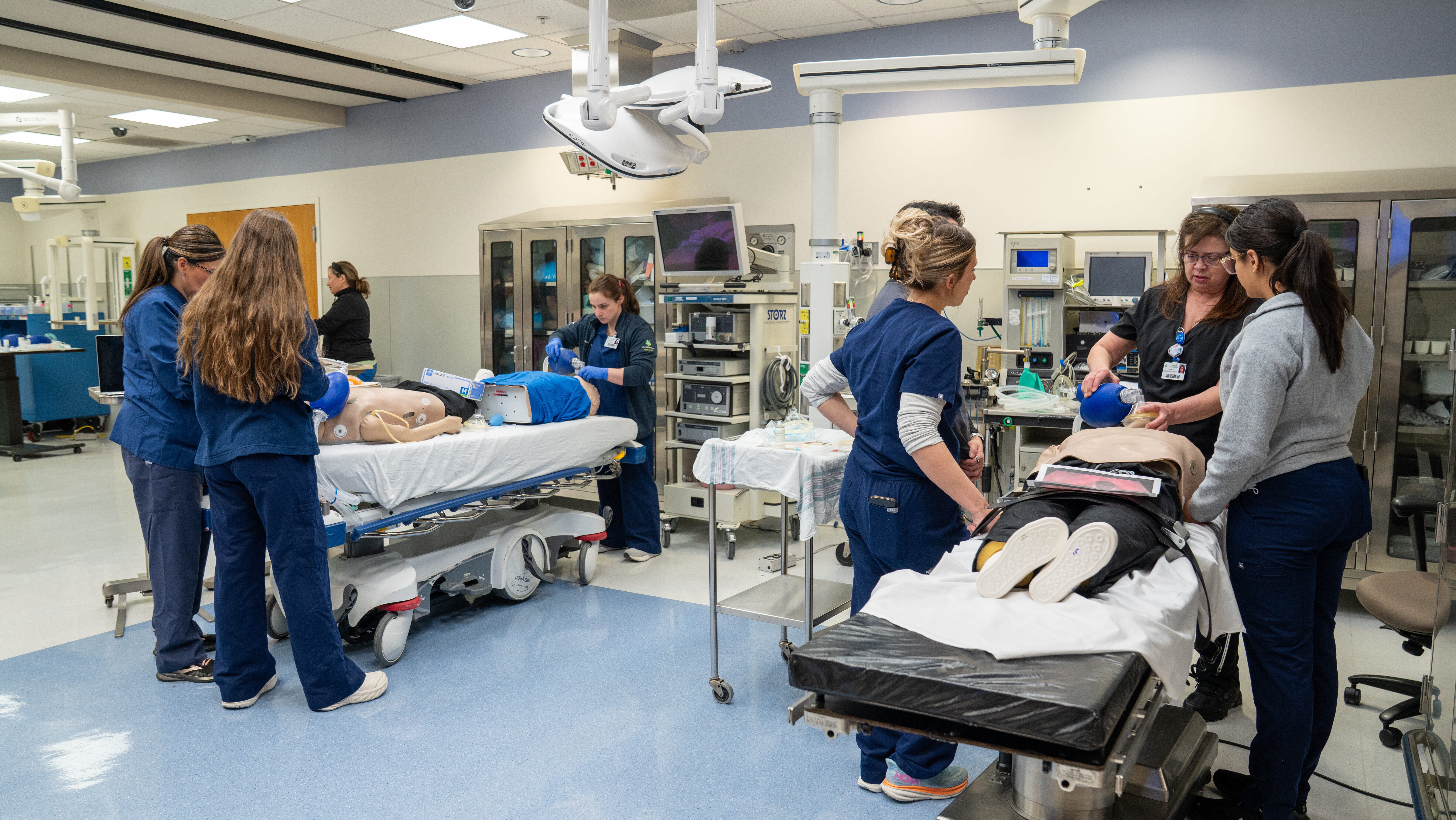
That morning in mid-February, Sorowice and her classmates rotated through a series of stations at ChristianaCare’s Virtual Education and Simulation Training (VEST) Center. They practiced mask ventilation, oral intubation using a laryngoscope, and other airway management techniques on high-fidelity manikins that mimic human anatomy and physiological response.
The VEST Center is a 9,000-square-foot facility on the Christiana Hospital campus, certified as a Level I Educational Institute by the American College of Surgeons and designed to replicate a working hospital environment, with a trauma bay, ICU, operating room and standardized patient rooms. Students in the nurse anesthesiology program are also using a virtual reality simulation platform called Simvana, which allows additional practice on airway skills and other competencies.
To design Delaware’s nurse anesthesiology program, Mainwaring spent more than a year working through the 152 national accreditation standards and building a comprehensive doctoral curriculum aligned with those standards. The curriculum integrates foundational sciences such as advanced physiology and pathophysiology, chemistry and physics as they relate to anesthesia practice, advanced anatomy, pharmacology, airway management, and comprehensive clinical assessment, along with specialty anesthesia content across the lifespan. Clinical education begins in the second year and progresses in complexity over the three-year program. In addition to extensive clinical training, students complete a doctoral practice project prior to graduation.

One feature Mainwaring built into the program intentionally is a strong emphasis on student wellness. She hired Matthew Zinder, DNAP, CRNA, a part-time faculty member who brings expertise in both nurse anesthesia and wellness science, to support this initiative. At orientation, families and partners are invited to a dinner centered on sustaining well-being throughout the program, reinforcing that support systems matter. The following day, students participate in a full-day wellness workshop designed to provide practical strategies for resilience, stress management, and performance under pressure. Her goal is to equip students with tools to both navigate the intensity of a three-year doctoral program and sustain a long, healthy career in a profession defined by high stakes and high responsibility.
Student Nadia Lazarczyk, RN, BSN, CCRN, had been a nurse in ChristianaCare’s surgical trauma ICU for nearly seven years. She was drawn to the nurse anesthetist path offering the same one-to-one intensity of the ICU, but with greater independence and scope. She had shadowed a CRNA in the operating room and realized it was the direction she wanted to go.
“I was drawn to nurse anesthesia because it combines advanced physiology, pharmacology and independent clinical judgment in a way that directly impacts patients in their most vulnerable moments,” Lazarczyk said. “That level of responsibility motivates me to grow and continually refine my clinical expertise.”
Both Sorowice and Lazarczyk have already signed contracts with ASPA to work at ChristianaCare after graduation. The program offers tuition assistance to prior ChristianaCare employees in exchange for a three-year post-graduation commitment, an arrangement that gives students financial footing and the region a pipeline it didn’t have before.
With the program now well underway, Mainwaring says that having students on campus has been the most rewarding part of the journey.
“Seeing our students in action is incredibly motivating,” she said. “They are, without question, the most important part of all of this.”