Drug overdoses claimed 64,000 American lives in 2016 — more lives than the AIDS epidemic at its height and up 22 percent from just a year before. In Delaware, 308 people died from overdoses in 2016, compared to 228 in the previous year.
“The opioid epidemic is a major catastrophe hitting our community,” said Terry Horton, M.D., FACP, FASAM, chief of the Division of Addiction Medicine and associate physician leader of the Behavioral Health Service Line at Christiana Care.
Heartbreaking stories of people who became addicted to prescription painkillers and then turned to cheaper heroin are all too common across the nation and in our local community. For all its tragedy, the national crisis also is awakening a greater understanding of addiction — and the strategies that are effective in addressing it.
“Addiction is a brain disease,” Dr. Horton said. Like other diseases, medical science offers tools that can help. Christiana Care Health System is a national leader in identifying and implementing these tools.
As Dr. Horton and his colleagues work to help patients in Delaware overcome their addiction, he also works to build understanding nationally about the nature of the problem and teaches others how to meet these challenges in their own communities.
At Christiana Care’s 5th Annual Addiction Medicine Symposium in August, more than 200 experts from psychology, law enforcement, government, treatment clinics and addiction medicine gathered to share information and learn about the ways that Christiana Care is successfully tackling the many facets of this public health challenge.
Christiana Care is adapting to the ongoing opioid crisis in its hospitals and in the community. This work includes a groundbreaking opioid withdrawal clinical pathway — featured recently on National Public Radio’s Morning Edition — which screens hospital admissions to find people going through withdrawal and connects them with resources to overcome their addiction. It also includes efforts to reduce opioid prescription, increase access to care, enhance care for infants and families impacted by opioids and much more.

Critical moments of intervention
When Austin Blanco recalls key life moments, like learning he was going to be a father and holding his son for the first time, he remembers exactly where he was: Christiana Hospital.
Since 2015, Blanco has been admitted three times for six-week treatments of a serious heart infection caused by intravenous drug use.
Now 23, he is clean and runs a landscaping business as he and his young family plan to build a new home in Middletown.
“I always said I wanted to achieve these goals, but to sit back and see them actually take off, it’s a lot different now,” Blanco said.
Blanco was one of the first patients to benefit from Christiana Care’s opioid withdrawal clinical pathway, which was piloted in four hospital units in May 2016 and launched systemwide the following November. This medical road map helps the hospital care team to better identify patients at risk for opioid addiction and guide them into effective treatment. Today, almost all patients admitted to the hospital are screened for withdrawal and evaluated for buprenorphine and discharge to a community provider.

“The hospital is a reachable moment,” Dr. Horton said. “With the right tools, methods and staff, we are able to help identify those with substance use disorders, engage them by addressing withdrawal and facilitate their transition to community-based treatment.”
Blanco recently returned to Christiana Hospital to visit with one of the people he credits with turning his life around: patient care facilitator Dori Barnes, BSN, RN-BC.
“I just wanted to do the right thing,” Barnes said. “I saw a kid, a young boy who deserved to get out of where he was.”
She and her colleagues were able to help him achieve that, using the processes and tools of the clinical pathway. Among them is a simple screening tool developed at Christiana Care that consists of two questions:
- “Have you used heroin or prescription pain medicines other than prescribed in the last week?”
- “Do you get sick if you don’t use heroin, methadone or prescription pain medications?“
“Most patients who know they will go through withdrawal answer yes,” said Patty McGraw, MS, BSN, RN, research coordinator for the Department of Medicine.
Patients who answer “yes” to either question are entered into the pathway and systematically evaluated using the Clinical Opiate Withdrawal Scale (COWS) to look for signs including restlessness, chills, flushing, tremors, runny nose, vomiting and diarrhea, which may indicate opioid withdrawal.
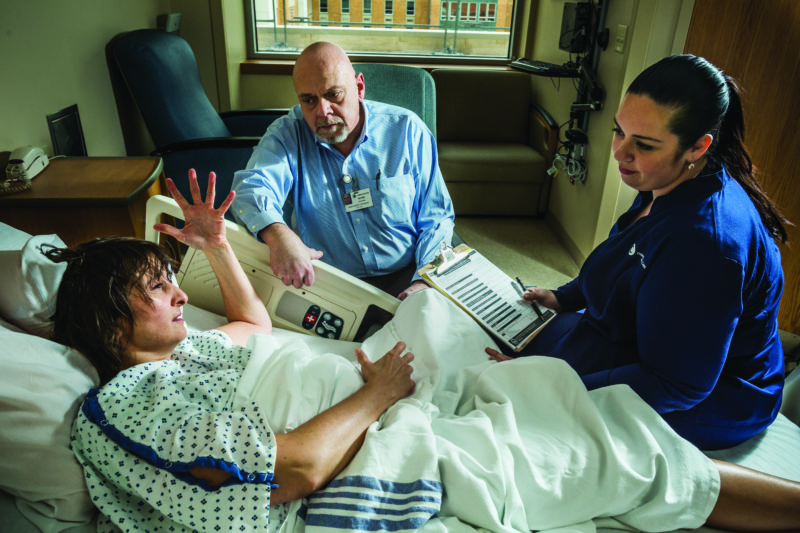
Christiana Care is validating the screening tool with an eye toward creating a national standard to help fight the country’s opioid epidemic.
Once identified, patients can be guided into medication-assisted treatment and therapy. Medication can relieve symptoms of withdrawal and prevent overdose deaths, and therapy can help address the trauma that is so often at the root of addiction.

“This is a population that oftentimes is very difficult to treat, not only for their medical complexity, but for the extraordinary challenges experienced during withdrawal,” said LeRoi Hicks, M.D., MPH, FACP, Hugh R. Sharp Jr. Chair of Medicine and physician leader of the Acute Medicine Service Line. “The best thing we can do is attend to their needs and provide comfort early on.”
He said that the work of the entire care team in developing this clinical pathway and providing the very best care to these patients is the embodiment of Christiana Care’s values — excellence and love.
“What’s been so rewarding about the process is the experience of working in this cross-disciplinary fashion, across service lines and in a unified effort to reduce variation in care for opioid withdrawal,” said Kimberly Williams, MPH, senior research associate at Christiana Care’s Value Institute. Williams and Claudine Jurkovitz, M.D., MPH, senior physician scientist in the Value Institute, designed the study protocol to validate the screening instrument and are supervising the analysis for the project.
Currently, staff screen about 70 percent of medical admissions. Largely through increased use of the opioid-replacement drug buprenorphine, Christiana Care has reduced 30-day hospital readmissions for opioid withdrawal by 30 percent. The health system also has standardized its discharge processes so that patients can be enrolled into long-term treatment in as little as 12 hours.
“It seems like it’s working. The potential for that is exciting,” said Beverly Wilson, MS, program manager for Christiana Care’s Project Engage, who co-led the implementation and development of the opioid withdrawal pathway. “There are very few that we’ve been aware of who have answered ‘no’ and gone into withdrawal.”
In May 2017, Dr. Horton testified before a U.S. Senate committee about combining medication-assisted treatment and therapy to combat overdose deaths.
“When we compare our results to other hospitals’ data, early outcomes of the pathway appear to show a reduction in the rate of patients leaving against medical advice,” Dr. Horton said. “We’ve been able to make an impact.”
Other health systems are noticing. In Huntington, West Virginia, a health system is working with Christiana Care to implement its own version of the pathway. Dr. Horton traveled to the city in August to help them address their opioid crisis and planned to return to West Virginia in December to deliver a grand rounds. West Virginia is among the states hit hardest by the opioid crisis.
“It’s greatly rewarding to know that the pathway we created here at Christiana Care is useful to others,” he said.
Medications key to overcoming addiction
The severity of opioid withdrawal is one of the main reasons that it’s so hard to quit. Opiates rewire the brain, and within hours after an addicted person stops using the drug, the brain responds with what Dr. Horton calls “primal misery.”
Thomas Bradford, MSW, a social worker with the Christiana Care Visiting Nurse Association, has heard much the same.
“The withdrawal is so painstakingly acute,” Bradford said, likening it to “horrible physiological agony.”
Often, an individual is faced with a choice between the agony of withdrawal and a cheap bag of heroin. But medication can stave off withdrawal and make that choice unnecessary.
A key part of the opioid withdrawal clinical pathway is consistent use of medications that mimic the neurological effects of opioids but without the accompanying intoxication.
Buprenorphine partially fills and blocks opioid receptors on neurons. It has about 40 percent of the effect of heroin, so it is much less likely to cause respiratory arrest and overdose death while alleviating the symptoms of withdrawal. When used daily, buprenorphine has been shown to reduce craving, opioid use and mortality.
Buprenorphine has been FDA-approved since 2003 but is still not used to its potential, Wilson M. Compton, M.D., MPE, deputy director of the National Institute on Drug Abuse, said at the symposium. In 2014, only 25 percent of opioid admissions included medication in their treatment plans. He said the government is looking to fund efforts that can increase use of these drugs, including through novel delivery solutions.
Dr. Horton said there is a misunderstanding, especially among the families of those with addiction, that buprenorphine treatment is just replacing one addiction for another. He tells them that addiction is a disease in which the victim takes drugs despite their negative consequences. With buprenorphine, patients avoid the myriad negative consequences of other opiates, most notably overdose and death.
He distills the data into a simple safety message for his patients: “Every day you take buprenorphine is a day you will not overdose and die.”
To their parents, he says, “We are in a dangerous epidemic. I know if your son or daughter takes their buprenorphine today they’re safe.”

Project Engage sets the standard
Christiana Care’s opioid withdrawal pathway grew out of a program called Project Engage, an early intervention and treatment-referral program designed at Christiana Care to help hospital patients who may be struggling with alcohol or drug use. Project Engage collaborates with hospital staff to identify and connect patients with community-based substance use disorder treatment programs and other resources. It was recently highlighted as a best-practice model by the American Hospital Association in the toolkit “Stem the Tide: Addressing the Opioid Epidemic.”
Project Engage was based on the understanding that patients who are in the hospital — even for reasons unrelated to addiction — are often at a low point and open to exploring treatment for their substance use. The program integrates peers in their recovery — called engagement specialists — who meet with patients at the bedside and help to mentor them through their treatment options.
In 2015, Project Engage formed a partnership with the construction industry to offer recovery support to employees from participating construction companies. The construction industry is second only to the hospitality industry for the proportion of workers who have an opioid addiction.
“It’s important for those with addiction to be able to acknowledge it,” said Stephen M. Mockbee, founder, chairman and former president of Bancroft Construction Company and a Christiana Care Health System trustee. He explains that a company is better off supporting those employees in their recovery rather than penalizing them. Of course, it’s unsafe for anyone under the influence to work a construction job. “But we give them hope to come back to their job if they’re clean,” Mockbee said.
“This is the right thing for employers to do, and it is the best option for the company, for the employees and for their families.”
Christiana Care is also working to partner with leaders in the Delaware hospitality industry on addiction recovery support for employees.

Tackling tobacco addiction
Project Engage’s innovative approach is proving remarkably successful in addressing many kinds of addiction — including tobacco. Through a program called Project Connect, Christiana Care is helping hospital patients to make the decision to quit smoking at a teachable moment — and connecting them with the resources to help.
Through the program, a tobacco treatment specialist meets with hospital patients for 20-minute interviews to discuss habits, motivation, home environment and past attempts to quit. Follow up may include post-discharge phone calls and, for those who are ready to quit, referrals to the Delaware Quitline or a face-to-face tobacco cessation coach at Christiana Care. Both services provide free tobacco-cessation medication.
A less intensive model of the project, which was piloted by volunteers, was recently honored with a 2017 Governor’s Outstanding Volunteer Service Award.
“Making the decision to quit is one of the best things you can do for yourself,” said Denise Taylor, MS, RD, Project Connect program manager. She reassures her patients, “It may be difficult when you get home and experience stressors and triggers to use tobacco, but we’re here to help you.”
Outpatient program reduces barriers to treatment
Christiana Care started an outpatient substance use program about two years ago due to demand for a multidisciplinary, integrated program that combines therapy with medications.
“We started out slow, and it grew quickly because the need is so substantial,” said Lisa Gonzalez, MS, LCDP, program coordinator.
The program’s niche is meeting the complex needs of patients suffering from addiction, including removing barriers to treatment such as transportation, access to health care and a variety of other stumbling blocks. It’s built for people for whom other options haven’t worked.
“Our program is about acknowledging that people often need extra help to succeed in treatment,” she said.
The program accepts referrals from within the Christiana Care network, including Project Engage, behavioral health and primary care. The team, which includes a dedicated social worker and counselor, is actively treating about 75 patients.
Gonzalez said alcohol remains the single most abused chemical, though most patients with addiction use multiple drugs.
Mental health therapy is the clinic’s baseline treatment; about half of its patients also take medication.
Jolomi Ikomi, M.D., joined the clinic as medical director in August after serving in the same role at a treatment clinic associated with the Yale School of Medicine. He said medication is sometimes appropriate to reduce cravings, which will ultimately make it easier to identify and treat underlying mental illness.
“If you address a patient’s withdrawal, then you can talk about the deeper psychological issues that have contributed to the addiction,” said Dr. Ikomi, a double board certified addiction psychiatrist. “There’s a lot of trauma among my patients.”
He said patients who take these drugs are able to begin to take steps to conquer their addiction in the long term.
“The majority of my patients feel gratitude and ask themselves why they did not get the medication earlier,” he said.
A minority of patients struggle with guilt.
“There’s a stigma of being on a medication, as people wonder if they are really in recovery if they are taking a drug,” he said.
He often tells patients the medication is not the cure.
“Really, what’s going to bring about change is counseling and psychotherapy,” he said.
Overall, Dr. Ikomi said the combination of medication and therapy has been shown to be effective.
Making progress on addiction, then, is largely about overcoming the barriers to this treatment, whether they’re financial, related to stigma or caused by provider hesitance.
Reducing opioid prescriptions
While prescriptions for opioids have been declining since 2010, the Centers for Disease Control reports that opioids are still overprescribed.
Two years ago, Christiana Care initiated a project to ensure all clinicians were adhering to opioid prescription regulations. Each primary care doctor in The Medical Group of Christiana Care was provided with a list of their patients receiving opioids for more than 90 days, and doctors reviewed their peers’ charts.
“We saw a reduction in the utilization of narcotics,” said Julie Silverstein, M.D., FACP, physician leader of Primary Care & Community Medicine. “The underlying goal is to make prescribing habits more thoughtful, to make sure that patients are aware of the risks and benefits of prescribing opioids.”
In April, Delaware passed requirements for opioid prescription that set new rules around written consent, urine drug screens, analyses of prescribing patterns and substantially limiting the quantities of medication that can be prescribed. Christiana Care collaborated in crafting this legislation. By November, Delaware reported a 12 percent drop in prescription rates statewide since the rules went into effect, as well as an 8 percent drop in the number of patients being treated with opioids.
Rethinking pain management
In his 2016 letter to physicians, U.S. Surgeon General Vivek H. Murthy, M.D., MBA, asked them to do three things to address the opioid crisis. In addition to pursuing evidence-based treatment and seeing addiction as a chronic illness, he asked providers to educate themselves about how to treat pain safely and effectively.
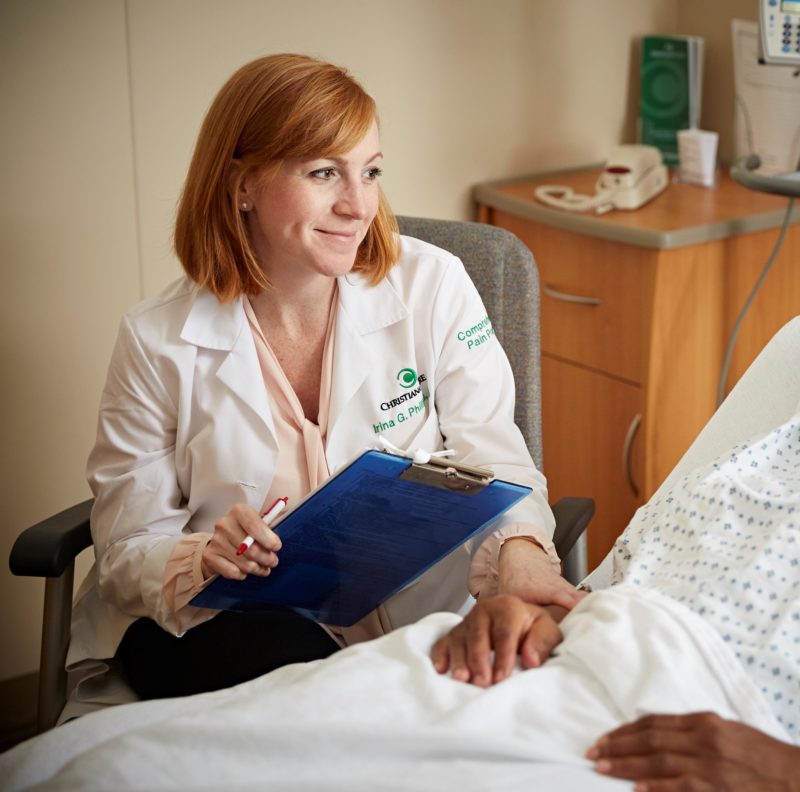
Irina Phillips, M.D., medical director of Christiana Care’s pain consult service, said providers were encouraged in the 1990s to treat pain aggressively. Early studies, though limited in scope, suggested opioids were safe for long-term use even in those without cancer.
“What began with good intentions led us into this difficult situation,” Dr. Phillips said.
Now, she’s working with complex cases at Christiana Hospital, including patients on opioid therapy for chronic conditions. Other cases include patients whose conditions make them vulnerable to the sedating effect of opioids and patients for whom the illicit use of injected drugs has led to consequences such as infections of the spine and heart.
“Most patients requesting opioid medication just want to feel better,” she said. Unfortunately, there is not solid evidence that long-term opioid therapy is effective. As patients build tolerance to the drugs, higher doses are required, which can be punishing to patients’ ability to function.
“The very thing they think is going to make them better we know won’t make them better,” she said. “A lot of patients don’t want to be on chronic opioids but can’t imagine any other way.”
Instead, Dr. Phillips pursues a multimodal pain strategy that may include non-opioid pain medications as well epidurals or nerve blocks. More often, medication is not the best solution, especially for the most common types of pain in the back and neck.
“For chronic back pain, we know the best relief is physical therapy and daily exercise,” she said.
The goal is not to relieve all of a patient’s pain, but to achieve a tolerable level of pain that allows patients to reach their goals.
“We’re turning our focus to preserving function, including in the hospital,” she said. For hospital patients, that could mean attending physical therapy or walking to the bathroom independently.
Achieving that function requires a personalized approach, including the patient’s substance-use history, toleration of medication and goals.
Advocating for access
The expansion of Medicaid in 31 states in 2014 as part of the Patient Protection and Affordable Care Act helped Delaware’s community providers expand access to substance-use care. This coverage is especially important in treating addiction, because the disease’s progression often inhibits the victim’s ability to work and receive employer-sponsored coverage.

“If you repeal and replace the Affordable Care Act in a way that impacts Medicaid in our state, including the potential for 40,000 or 50,000 people to come off Medicaid rolls, you will remove the access to what is effectively life-saving treatment,” said Bettina Tweardy Riveros, Esq., Christiana Care’s chief health equity officer and senior vice president, government affairs and community engagement.
Throughout the past year, Christiana Care has been engaged with community leaders and government officials to help preserve access to care for people struggling with addiction. These efforts included successful state legislation that requires insurance companies and Medicaid plan participants to cover treatment for substance-use disorder.
Infant victims of addiction
As Delaware’s leading maternity hospital, delivering more than 6,000 babies every year, Christiana Care is at the forefront in caring for infants who are exposed to drugs in the womb — and their families.
Infants who experience withdrawal after birth need their mothers more than anything else. Time spent together cements a bond and calms the infant, dampening the effects of withdrawal. Their mothers need something else altogether: acceptance. Already stigmatized for their addiction, they are quick to sense the judgment, overt or subtle, of their health care providers.

Though doctors teach that addiction is a chronic disease and not a choice, the public is often inclined to demonize parents who struggle with addiction. This attitude is hurtful to parents but ultimately does the most damage to the infants, said David A. Paul, M.D., chair of the Department of Pediatrics and clinical leader of the Women and Children’s Service Line.
“In order to solve this problem and care for infants, we have to care for the families,” Dr. Paul said. “If you blame the mother for causing the baby’s illness, then the parents pick up on that. If parents don’t feel welcome, they’re not going to be there as often. We need to have the parents engaged, and we need the moms breastfeeding and learning to take care of their infants.”
Christiana Care cares for about 200 infants a year who are exposed to opioids before birth. These infants develop neonatal abstinence syndrome, or NAS, which is essentially a set of short-term withdrawal symptoms with unclear long-term consequences.
Christiana Care has created a medical regimen that weans infants off opioids in the hospital and helps parents adjust to their new responsibilities. Christiana Care also has consolidated comprehensive services — including addiction psychology, midwifery and social services — into a pregnancy support center in Wilmington Hospital that opened in September.
“We want to be able to give our patients the ability to have on-site, wraparound services,” said Elizabeth M. Zadzielski, M.D., MBA, FACOG, associate physician leader of the Women and Children’s Service Line.

Some infants undergoing withdrawal face complex medical needs that require care in Christiana Hospital’s Level III neonatal intensive care unit (NICU). For babies who don’t require intensive care, Christiana Care created a special unit called the Continuing Care Nursery that serves the special needs of infants who are experiencing withdrawal and their families. The unit has a quiet environment and single-family rooms. Parents are encouraged to stay with their infants as much as possible.
Christiana Care also has a volunteer Cuddlers program that helps to provide comfort and human contact for babies when the mother is not present.
Infants with NAS cared for in the Continuing Care Nursery stay at the hospital for 11 fewer days compared with infants with NAS who are treated in the NICU. Though it’s possible that the severity of infants’ medical complications in the NICU is partly responsible for their longer stays, Dr. Paul believes the calmer, family-centered environment of the Continuing Care Nursery is the causal factor.
When these infants are released from the hospital, they are no longer dependent on opioids, and their withdrawal symptoms have eased, but the illness is not over. They can display symptoms for months. Nurses from Christiana Care’s Visiting Nurse Association play a key role in helping both mother and baby stay on track.
Jennifer Velasco, BSN, RN, has been conducting home visits for 25 years. She said infants with NAS were once rare but now account for more than half of her cases.
“We offer a crucial service for these new moms,” Velasco said. “They’re not in the hospital anymore with eyes on them 24/7.”
Her colleague, Kathleen Brady, RN, said giving birth is often a major turning point for mothers who are addicted to opioids.
“They realize the seriousness of their condition and the need to have treatment,” Brady said. “They’re very motivated to care for their baby and do the right thing.”
Forming a mother-child bond is essential in the weeks and months after hospital discharge. The symptoms of NAS — especially irritability and difficulty focusing on parents — can make this bond more difficult to form. The nurses teach parents how to massage their infants and calm them with skin-to-skin contact. They also evaluate the safety of the home and the readiness of the parents.
If the child is gaining weight and appears healthy, two visits are often sufficient. Fortunately, the long-term effects of NAS do not appear to be as severe as with fetal alcohol syndrome.
Still, Dr. Paul said it’s unclear what the long-term effects of NAS might be, largely because it’s difficult to isolate the relative impact of opioids, other substance exposure and sociological risk factors after birth. A child’s environment growing up is likely more determinative of their lifelong health than the drug exposure in utero, he said.
Addressing these social and environmental, rather than medical, determinants of health will remain a major challenge.
“Our goal is to keep mothers off illicit drugs and to give them the framework and support they need while pregnant and beyond,” Dr. Zadzielski said.



