Facts about Zika
Questions and answers about the Zika virus
Marci Drees, M.D., MS, FACP, DTMH, infection prevention officer and hospital epidemiologist for Christiana Care Health System, provides information on the Zika virus.
Q: What is Zika?
A: Zika virus disease is caused by the Zika virus, which is spread to people primarily through the bite of certain infected mosquitoes. Most people with Zika virus do not have symptoms at all, and among those who do, the illness is usually mild, with symptoms including fever, rash and conjunctivitis (pink eye) lasting up to a week. However, Zika virus infection during pregnancy can cause microcephaly (small head) and other severe brain defects in the infant. Guillain-Barre syndrome, an uncommon sickness of the nervous system, can be triggered by Zika in a small number of cases.
Once someone has been infected with Zika, their immune system may protect them from future infections. There is no evidence that past Zika infections pose an increased risk of birth defects in future pregnancies.
Q: What are the symptoms of Zika virus disease?
A: The most common symptoms of Zika virus disease are fever, rash, joint pain and red eyes. Other symptoms include muscle pains and headaches. Many people infected with Zika will have only mild symptoms, which can last for several days, or none at all. Other diseases, such as dengue and chikungunya, which are transmitted in the same regions of the world, may have similar symptoms.
Q: Where is Zika virus?
A: Zika virus has been identified in humans living in more than 50 nations, but it is most commonly found in South America, Central America and the Caribbean region. A list of the affected countries is continuously updated on the website of the Centers for Disease Control and Prevention. In these areas, most transmissions to humans occur through mosquito bites. Nearly all U.S. cases of Zika have been related to travel to high-risk areas and have occurred through mosquito bites.
Recently, a neighborhood in Miami, Florida, has experienced a small number of mosquito-borne infections and, as a result, Florida health officials are actively targeting mosquito populations with insecticides.
At this time, there have been 10 cases identified in Delaware, all related to travel. There has been no Zika virus identified in Delaware mosquitoes to-date.
Q: How do people get infected with Zika?
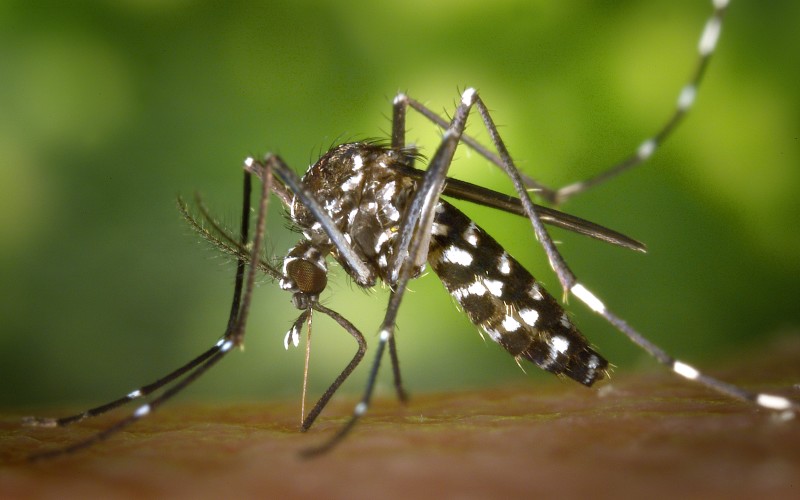
A: Zika is spread to people primarily through the bite of an infected Aedes species mosquito. These are mosquitoes that live in urban environments and primarily bite during the day.
A pregnant woman can pass Zika to her fetus during pregnancy or around the time of birth. Transmission also can occur sexually. People who have traveled to places where Zika has spread or live in places where Zika has been identified should protect themselves by preventing mosquito bites and practicing safe sex. More details about precautions may be found on the CDC website.
Q: How is Zika diagnosed?
A: To diagnose Zika, your doctor will ask you about recent travel and about symptoms you may have, and collect blood or urine to test for Zika or similar viruses.
Q: Should pregnant women travel to areas where Zika has been confirmed?
A: No. Pregnant women should not travel to any area with active Zika virus transmission. If such travel cannot be avoided, the woman and her sexual partner should discuss the risk of Zika infection and how to prevent it with her doctor. Both the pregnant woman and her sexual partner should strictly follow steps to prevent mosquito bites. If a pregnant woman’s partner travels to a Zika-affected area, they should use condoms or not have sex (vaginal, anal or oral) during the pregnancy. Women who are trying to become pregnant should discuss with their doctors, prior to travel, their plans to become pregnant and the risk of Zika infection. Refer to CDC for guidance on how long you should wait to get pregnant after traveling.
Q: What can people do to prevent Zika?
A: The best way to prevent Zika is to protect yourself and your family from mosquito bites:
- Use Environmental Protection Agency registered insect repellents, such as DEET. Delaware health officials recently announced that Medicaid now covers mosquito repellent.
- Wear long-sleeved shirts and long pants.
- Sleep in areas that have closed doors and screens. Air-conditioned areas are preferred.
- Zika also can be spread sexually. People whose sex partners have traveled to or live in an area with Zika can prevent Zika by using condoms or other barriers every time they have sex (vaginal, anal or oral) or by abstaining from sex.
Q: Can someone who returned from an area with Zika get tested for the virus?
A: People who have symptoms of Zika – or who have returned from areas that have high rates of Zika infections – should be tested. People without symptoms (other than pregnant women) do not require testing. The CDC provides guidance for Zika virus testing with state public health laboratories. The Food and Drug Administration (FDA) recently has issued an Emergency Use Authorization for qualified commercial laboratories to provide testing. Widespread testing is not recommended at this time.
Q: What should pregnant women who have recently traveled to an area with Zika do?
A: Pregnant women who have recently traveled to an area with Zika should discuss their travel history with their doctor, regardless of whether they are sick.
Q: Can anyone get tested for the Zika virus?
A: Widespread testing is not recommended at this time. All pregnant women should be assessed at prenatal visits for Zika virus exposure (either through travel or by sexual contact with an individual who traveled to an area with Zika virus) and get tested if there is exposure. Men or women who have been exposed through travel or sexual contact and have symptoms of Zika virus infection (e.g. fever, rash, conjunctivitis) should be tested.
Q: Can anyone request a Zika virus test?
A: Consult your health care provider if you have questions or think you should be tested. The CDC has specified that laboratories in the United States should limit testing of specimens to those collected from patients meeting CDC’s clinical and epidemiological criteria for testing. Information on clinical signs and symptoms associated with Zika virus infection is available on the CDC’s website. It is important to note that Zika virus infection can cause signs and symptoms similar to those seen in patients with dengue and chikungunya virus infections, and testing for those infections may be recommended as well.
Q: Should I be concerned about getting a blood transfusion?
A: Zika virus poses a low risk to the blood supply in the continental U.S., but this could change depending on how many people become infected with the virus. In Brazil, there have been cases of people who contracted Zika through blood transfusions. In the United States, recent travelers to Zika-affected areas are asked not to donate blood for a period of time, even if they do not have symptoms. In areas of active transmission, the FDA recommends that blood either be screened by laboratory testing, subjected to pathogen-reduction technology or outsourced from other areas. The FDA continues to monitor this potential outbreak in cooperation with the CDC and Florida State public health officials.
Q: If I am going to get a blood transfusion, do I need to have the blood tested for Zika to ensure the blood is safe from Zika?
A: In the United States, the blood supply is considered safe because there is not an ongoing transmission of Zika virus and because travelers are screened for possible Zika exposure and not allowed to donate if they have recently traveled. The FDA continues to monitor the situation and will start screening the blood supply if that is deemed necessary.
Q: Can Christiana Care test for Zika virus?
A: Christiana Care’s laboratory staff continues to work with the Delaware Division of Public Health Laboratory to ensure all patients in need of Zika evaluation are able to be tested.
This article was originally published on Feb. 16, 2016, and was updated on Aug. 9, 2016.