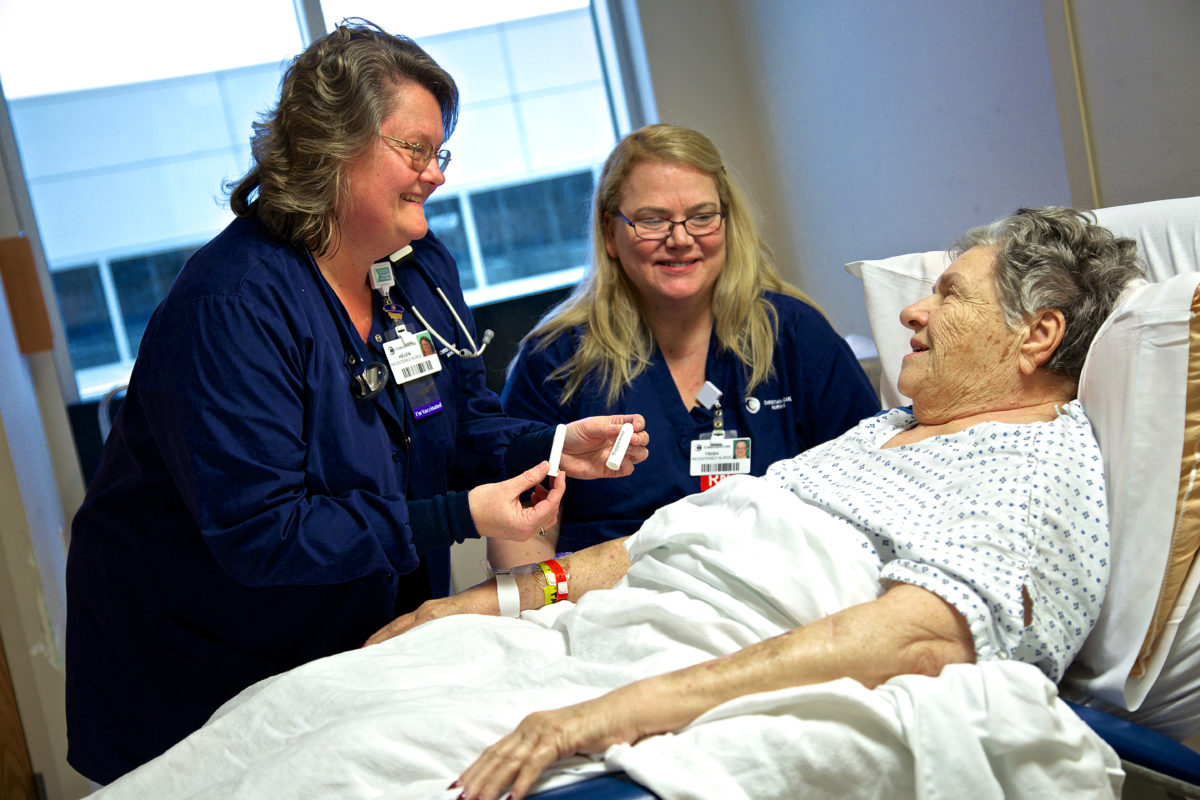
Cardiovascular Critical Care Unit (CVCCC) nurses Helen Hawrylack, BSN, CCRN, RN III, and Patricia Briggs, MSN, RN IV, CCRN, HTCP, HTI/1, are always looking for ways to improve their patients’ experience and get them involved in their own health care.
In 2013, they found an article on treating nausea in post-operative patients using a nasal inhaler suffused with peppermint oil.
“We couldn’t find anything particularly addressing its use with open-heart surgery patients,” Hawrylack said. At the same time, they were looking for an opportunity to do a simple study that would engage the nursing staff in research. So they purchased inhalers and peppermint oil and embarked on a study — one so successful that the surgeons in their unit immediately adopted the practice to relieve patients’ nausea.
“Just giving them the inhaler made patients feel they had more control over their care, and it was easy for nurses to incorporate into their routine,” Hawrylack said. “We had patients asking to take the inhalers home.”
Today, the devices are available throughout Christiana Care Health System.

The pair presented their findings at American Association of Critical Care Nurses National Teaching Institute & Critical Care Exposition in New Orleans in May 2016, and the study will publish in the June issue of the journal Nursing 2016.
“We’ve used the study as a teaching tool for nurses who are making and presenting posters, and mentored two nurses in writing one of the two articles that will be published in Nursing 2016,” said Hawrylack.
According to Nursing Research Facilitator Lynn Bayne, Ph.D., NNP-BC, soon after the study began in the CVCCC, news of its success began to spread. “Before you knew it, the people in the next unit wanted to do it and get trained on it,” Bayne said. “What we realized was there was this strong body of knowledge out there that suggests that peppermint is an effective anti-nausea agent. It’s been in the literature a long, long time.”
The study’s findings were striking. Among participants, 93 percent said they were satisfied with the inhaler’s effectiveness and would use it again.
The new procedure for the use of peppermint inhalers was approved by the Systemwide Evidence-Based Nursing Practice Council in May 2015. The target areas for its use are in pregnant women, patients waking up from anesthesia, those undergoing joint replacements and people with colitis.
“The goal is that in the next year, we will be taking the research work and modeling it into a bundle of performance-improvement initiatives,” Bayne said. “The ultimate goal is for it being a first-line therapy that you would offer to a patient.”
If the inhaler is going to be effective in a patient, it will work in two minutes, Hawrylack said. If it’s not, a patient can be prescribed Zofran, a pharmaceutical alternative, which takes up to 44 minutes to kick in.
The peppermint inhalers are less expensive than pharmaceutical options and have no side effects. They can be given to a patient of any age, and they can use it as often as they wish.
“You’re letting the patient have control over their symptoms instead of having to buzz the nurse and ask for Zofran, and having the nurse say, ‘I’m sorry, Mr. Smith, it’s written for every six hours and it’s not time yet.’ There’s no such thing as an overdose of peppermint oil,” Bayne said.