Neurointerventional surgery enables treatments that might have seemed miraculous only decades ago
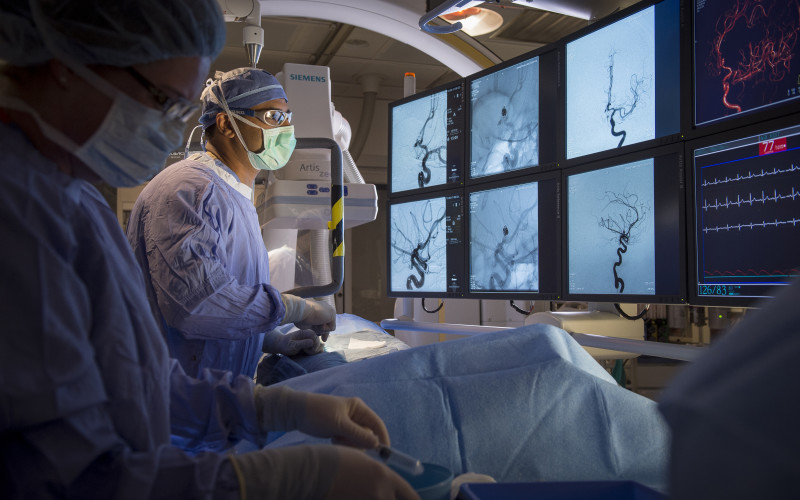
Advances in neurointerventional surgery allow treatment of potentially deadly brain aneurysms and some patients with acute ischemic strokes, which previously were untreatable or only treatable with open surgery. Christiana Care’s elite specialists in the field are taking full advantage of the state of the science.
Today, a patient having a stroke due to an acute blood clot in the brain or a ruptured brain aneurysm can receive the same level of care at Christiana Care that only a few years ago would have required a trip to a major teaching hospital in another state.

Gregg Zoarski, M.D., a neurointerventional radiologist who joined Christiana Care in 2011 with more than 20 years’ experience, describes one patient’s history that he says illustrates how the discipline has advanced:
About 12 years ago at the University of Maryland, Dr. Zoarski was involved in caring for a woman who had a giant right intracranial internal carotid artery aneurysm — a condition where a main artery supplying blood to the brain had developed a “bubble” due to a weakened arterial wall. The aneurysm was “the size of a tangerine” and had to be surgically bypassed, he said.
Complicating the case, “the patient also had a large left-side carotid aneurysm,” although it was not as large as the right side, Dr. Zoarski said. Having bilateral aneurysms — affecting left and right carotids — increased the risk for complications during surgery due to too little blood supplying her brain as the flow from the right had to be stopped to effect repairs.
The woman’s aneurysm was successfully treated with open surgery and bypass, but she sustained complete blindness in her right eye after surgery.
“The past 10 years have been marked by rapid evolution and increasing options in treatment of neurovascular diseases.”
A few years later, the left-sided aneurysm began to grow, and the patient began getting worsening headaches and losing vision in her other eye. Dr. Zoarski was able to offer her a new option: a minimally invasive procedure using endovascular coiling, where soft metal threads (platinum coils) are placed inside the aneurysm through the blood vessels from the right groin. She chose the minimally invasive option, with good initial success, but the aneurysm returned because of the large size and shape of the opening into the sac.
Last year, Dr. Zoarski and his patient turned to another new option, the Pipeline embolization device, recently FDA approved and acquired by Christiana Care in 2013.
“The device changes the flow of blood into the aneurysm and allows natural clotting along the weakened blood vessel wall,” Dr. Zoarski explained. Ultimately, the aneurysm clots and gets resorbed by the body.
Within weeks of the procedure with the flow-diversion device, the patient’s eye pain and vision improved. “She’s got complete and permanent occlusion of the aneurysm now, and beautiful reconstruction of the carotid artery,” Dr. Zoarski said. “We went from a surgical procedure 12 years ago that left her partially blind to an interventional procedure four or five years ago on the other side that left her with an incomplete result and a recurring aneurysm. Then last year, using the newest devices, we were able to get complete occlusion. At one year follow-up, her vision in the left eye is markedly better, and her headaches have completely resolved. The past 10 years have been marked by rapid evolution and increasing options in treatment of neurovascular diseases,” he said.

Seven years ago, Cleveland Clinic-trained Barbara Albani, M.D., arrived in Delaware to establish Christiana Care Neurointerventional Surgery. At the time, no complex cerebrovascular work was being done in Delaware. “Today Christiana Care offers full-service cerebrovascular care in conjunction with our collegues in neurocritical care, stroke neurology and neurosurgery,” Dr. Albani said.
Before 2007, “treating acute strokes caused by blood clots to the brain were limited to injecting the blocked blood vessel with tissue plasminogen activator — tPA — to try to dissolve the clot. We did not yet have the technology to go in and fix the problem. Since 2007, there have been five FDA-approved devices for the treatment of acute ischemic stroke (strokes caused by blood clots).”
When Dr. Albani started the neurointerventional program, she said, her first goal was to care for the stroke population that had no local opportunity for intervention. In many patients, because stroke treatment is time-sensitive, patients would often not receive any interventional treatment. “The program expanded from there, including an increased volume of emergent and elective brain aneurysm cases,” she said. “We’re meeting what otherwise was an unmet need in our community. That’s good, because the volume of stroke patients has exploded.”
Sudhakar R. Satti, M.D., joined Christiana Care Neurointerventional Surgery in October 2010. In the time since his arrival, “We have gone from treating two people with strokes in a year to now treating almost one acute stroke patient a week,” he said. “This dramatic increase in the number of patients treated is multifactorial, but can be largely explained by the commitment of Christiana Care to serve the community and to build a top-notch neuroscience program.” He credits the leadership of Timothy J. Gardner, M.D., medical director of the Christiana Care Center for Heart & Vascular Health.
In the past year and a half, Dr. Satti has used the Pipeline embolization device more than 20 times. He and colleagues Zoarski and Albani are listed among only about 110 doctors certified by the FDA to use the devices.
Christiana Care has a state-of-the-science facility dedicated to neurointerventional procedures. The program has a Neuro Intensive Care Unit with 24/7 coverage by five board-certified neurocritical care physicians and seven neurosurgeons. A dedicated stroke neurology team is currently being developed.
“We have everything that a high-level academic program would have, with the exception of residents and fellows,” Dr. Albani said. “Being able to provide world-class care closer to home is a big help to patients and their families.This becomes even more important as many neurovascular patients require lifelong follow-up and long-term care.”