Christiana Care Health System is poised to roll out new clinical pathways designed to reduce unnecessary variation in care and optimize the health and experience of patients with certain conditions and diseases. Pathways will help doctors, nurses and other care providers to implement comprehensive, individualized care plans for their patients using the most up-to-date information and connections to resources in the community.
Clinical pathways are like the familiar recipes you’ve made time and again from memory — but it takes just that once to forget a step, said Kenneth Silverstein, M.D., MBA, chief clinical officer.

“Even if you’re sure, if every time you made those chocolate chip cookies you used a checklist, you would never fail,” Dr. Silverstein said. “We don’t have the luxury to fail in this business. In a high-stakes environment, you want to have prompts so that you’re not missing anything. You don’t want to rely on memory.”
Each clinical pathway provides a road map to guide patients to an optimal health outcome, engage them as partners in their care and connect them with the follow-up services they need to manage their condition. A typical pathway might include algorithms for screening, evaluation, diagnosis and treatment, answers to common questions or concerns that patients might have, recommendations for appropriate patient-education materials, information about services and resources available to patients and their families, and recommendations for follow-up and preventive care.
Christiana Care’s nine service lines will each launch one clinical pathway this year. Development of additional clinical pathways is planned to develop exponentially in coming years, with new pathways added and existing pathways updated on a continual basis. This effort is a key component of Christiana Care’s strategy to achieve its aims of Optimal Health, Exceptional Experience and Organizational Vitality.
Development of the pathways has been the work of Christiana Care’s nine service lines: Acute Medicine, Behavioral Health, Cancer, Heart and Vascular, Musculoskeletal Health, Neurosciences, Primary Care & Community Medicine, Surgical Services and Women’s & Children’s.
The initial guidelines set the stage for development of an ever-expanding library of pathways that will enable consistent, evidence-based care across the continuum for a diverse variety of conditions.
The first nine pathways will initially be rolled out internally, but the goal is to quickly make them available to clinicians and care providers throughout the community on an easily accessible website. An implementation team is coordinating education, communication and IT efforts to support the rollout.
Although a care delivery model may be standardized as a clinical pathway, the way it is applied to each patient is personalized.
“This is simply about embracing patients and being a better partner with them. It’s about taking care of people – the pathways are just a tool for this,” Dr. Silverstein said.
The diseases chosen by the service lines range from Stage 2 non-small-cell lung cancer, which affects about 35 patients per year, to Type 2 diabetes, for which Christiana Care sees about 25,000 people annually.
What the pathways have in common is their potential to make a positive impact on people’s lives — and to inform the development of future clinical pathways.

“When you reduce variation, you achieve better outcomes for your patients,” said Mike Eppehimer, MHSA, FACHE, senior vice president for service line operations. “Being able to give patients a more predictable pathway and engaging them as partners in their care will improve overall patient experience because they’ll understand what’s happening now, what’s happening next and what their role is.
“The final piece is the value equation. Organizations that reduce variation and improve their outcomes also save costs. We’re not doing it for the financial incentive, but it does benefit organizational vitality.”
The service lines have begun rolling out pieces of the first nine pathways, with full pathway implementation to continue through the end of June. After that, new pathways will be developed each year and existing pathways will be continually updated.
“It’s amazing how much work the teams have gotten done. We are doing this very rapidly,” Eppehimer said. “There’s a tremendous amount of momentum around these pathways, an energy around it that makes it different from anything we’ve done in the past.”

Acute Medicine: Chronic obstructive pulmonary disease
Chronic obstructive pulmonary disease, or COPD, is the fourth-leading diagnosis among patients admitted to Christiana Care, accounting for about 1,200 hospital admissions each year. While the number of people who smoke – the main risk factor – is stable, the prevalence, how many people have COPD, is increasing, said Vinay Maheshwari, M.D., FCCP, associate chair for specialty medicine for the Department of Medicine and associate operations leader for the Acute Medicine service line.
This prevalence was one of the reasons the Acute Medicine service line chose COPD as its initial clinical pathway. In addition, the health system has had ongoing initiatives for the past few years to reduce the length of stay and readmissions related to the disease.

“We realized there were a lot of gaps in care and an opportunity to improve care coordination inside and beyond the hospital walls,” said Fran Gott, MBA, RRT, administrative director of pulmonary services and medical critical care. “Our 30-day readmission rate showed we had room to improve compared with the national standard.”
The first step is building a care coordination team that will optimize the multidisciplinary care of patients in the hospital and provide a standardized pathway for their follow-up after discharge. The team will be a resource for providers outside of the hospital to ensure that all the elements of care are being delivered.
“In today’s world we work in silos, all aimed at doing the right thing, but not always in the most coordinated fashion,” said Dr. Maheshwari. “We need to become really good at, while the patient is here in front of us, connecting the patient with all the services beyond the hospital walls, like smoking-cessation classes. We also need to assess other areas, such as the availability of home health care and making sure they can afford their medications. The biggest piece is post-acute-care hospitalization follow-up.”
Patients who meet certain criteria will be followed 90 days after leaving the hospital through Christiana Care’s CareVio service, Gott said. The service line is also considering creating a post-discharge clinic as a one-stop shop for COPD patients to get follow-up in the immediate post-hospitalization period.
“Those who check on patients can see if they’re having new or different symptoms and address them in a proactive way at home instead of waiting for the patients to show up in the emergency room,” he said. “Our hope is that, for example, if we have a patient and there are five things that need to happen, CareVio can check in and say, ‘Did you do X? Did you see Y?’ Then CareVio can tie the patient in to a provider so things don’t snowball.”
At the core of the effort is education — of patients and providers.
“The level of engagement we want from patients themselves is increasing,” Dr. Maheshwari said. “Patients will be getting literature that mirrors that of the providers: Here’s what you should be doing on day one. You should feel better by this time. Here’s where you should be making changes in medication.”
Said Gott: “It’s really standardizing evidence-based best practices. By embedding the GOLD guidelines (Global Initiative for Chronic Obstructive Lung Disease) in our pathway, we should be providing the latest and greatest care for COPD patients.
“Having a standardized focus around COPD will make it a better experience for patients. While they’re here they’ll be educated and, more importantly, they will be connected to the services that hopefully will make their daily lives more enjoyable. The ultimate goal is to improve their quality of life.”

Behavioral Health: Opioid addiction
The focus of Behavioral Health’s clinical pathway reflects a state and national epidemic: opioid addiction.
Specifically, the service line is working to standardize the screening, identification and treatment of patients at risk of opioid withdrawal.

“It’s really part of a bigger effort to integrate behavioral health into health care,” said Terry L. Horton, M.D., FACP, chief of the Division of Addiction Medicine and medical director of Project Engage, and associate physician leader for the Behavioral Health service line.
“There’s no standardized method to identify or care for these individuals, and there’s not a standardized care pathway,” he said. “You can have a lot of variations, some of which are not clinically sound or effective. It creates a terrific opportunity for improvement.”
That variation in care, as well as untreated withdrawal, increases the number of patients who sign themselves out against medical advice (AMA). It also increases the length of hospital stays, readmissions and the cost of care. And it results in poor patient experience, low staff morale — and even safety issues when patients engage in illicit drug use while hospitalized.
At the heart of the challenge is that such patients generally show up at the Emergency Department for other medical issues, like pneumonia or infections, and don’t self-identify their opioid use.
The first step, then, will be to implement a screening tool, which is being developed in partnership with the Christiana Care Value Institute.
“We will need to assess this with rigorous science,” he said.
The effort, Dr. Horton said, is directly analogous to Christiana Care’s adoption of Alcohol Withdrawal Risk Evaluation and Treatment Guidelines, which in 2012 were recognized by the Agency for Healthcare Research and Quality.
“There’s a lot of mythology out there that opioid withdrawal is not life-threatening, as opposed to alcohol withdrawal,” Dr. Horton said. “The reality is it can be as lethal.”
Just as patients at risk for alcohol withdrawal undergo the Clinical Institute Withdrawal Assessment, those identified as opioid users will be monitored using the Clinical Opiate Withdrawal Scale.
That monitoring will be linked with a computerized order entry system to help manage their symptoms.
“One thing we’d like to see is that more individuals are being identified with opioid dependence or opioid withdrawal,” said Dr. Horton, noting that today there are no firm statistics of opioid use in Delaware. The Centers for Disease Control and Prevention estimate that nearly 1 percent of any population is opioid-dependent, which could mean 8,000 Delawareans. Generally, fewer than 10 percent of those afflicted are in treatment. That could translate to anywhere from 2 percent to 10 percent of hospital admissions, said Dr. Horton, adding that the pathway should help to quantify the population.
“We appreciate that opioid use is a worsening epidemic,” he said. “Fatal overdoses have gone through the ceiling.”
The pathway aims to optimize health care outcomes and patient experience by treating at-risk patients effectively with medicine, reducing the AMA rate and readmissions, enabling patients to complete treatment and subsequently connecting them to proper community-based care.
“I’m very encouraged that we’re going to work on these issues, which are part of our community and haven’t been actively addressed,” he said. “We’re going to be pioneering efforts that can be replicated throughout the country.”

Cancer: Operable Stage 2 non-small-cell lung cancer
Clinical pathways aren’t a new concept in cancer care, which has been following standardized guidelines for more than three decades, according to Nicholas Petrelli, M.D., Bank of America endowed medical director of the Helen F. Graham Cancer Center & Research Institute and physician leader for the Cancer Care service line.
He expects that his thoracic team already is 80 percent compliant with the clinical pathway the group has developed to focus on operable Stage 2 non-small-cell lung cancer.
In Delaware and the United States, lung cancer is the most frequently diagnosed form of cancer, and it’s the most common cause of death from cancer. The Helen F. Graham Cancer Center & Research Institute sees about 35 patients with Stage 2 non-small-cell lung cancer each year.

“This gives us an opportunity to take a hard look at the treatment of those patients,” Dr. Petrelli said. “We started with a clinical pathway where we weren’t going to be overwhelmed with a lot of patients and an inability to monitor compliance.”
The patients are a homogeneous population, said Jamil Khatri, M.D., Quality Partners leader for the service line. Stage 2 non-small-cell lung cancer has more of a defined treatment protocol for the condition than for other stages of the disease, he said.
Dr. Petrelli said the providers will be following patients as they normally do. But, he said, “Now they have a defined pathway to follow, and we will be focusing intensely on the guidelines. We may find opportunities to improve processes of care.”
Dr. Khatri added that while they are addressing a narrow population, there is still some variation in care that the group will be measuring — for example, in tests ordered, surgical procedures done and follow-up care.
It will be critical to monitor compliance only in those areas of the pathway for which we can collect accurate data, according to Christopher D. Koprowski, M.D., associate service line leader and chair of the Patient Quality & Safety Committee of the Graham Cancer Center.
Among the pathway’s goals are decreasing the number of imaging procedures from diagnosis through survivorship and reducing the cost of care by standardizing chemotherapy protocols.
Because survival improves with early diagnosis, the group also will be increasing screening to find earlier-stage cancers. And because 85 percent to 90 percent of lung cancer is caused by tobacco use, they will be encouraging smoking-cessation programs.
One of the biggest efforts within the pathway will be increasing communication with primary care physicians.
“That will be one of the key elements: How do we bring the primary care provider into the pathway? Where do we bring them in, and how do we improve communication?” Dr. Petrelli said.
The service line also is developing a roadmap for patients that will mirror the clinical pathway so they can become engaged in the process of their own care.
Once this first clinical pathway is up and running, Dr. Petrelli said, the group will be replicating the effort with breast, colorectal, pancreas and prostate cancers.
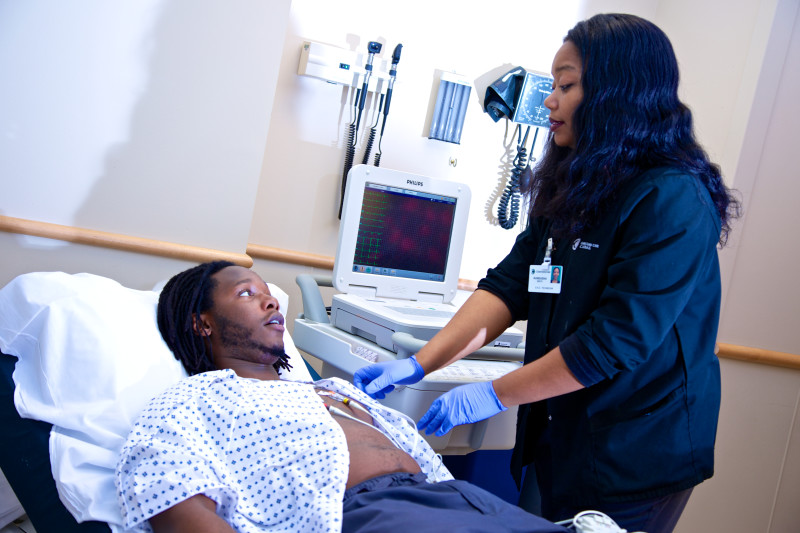
Heart and Vascular: Non-ST-segment-elevation myocardial infarction
Patients suffering the most common type of heart attack will be the beneficiaries of the clinical pathway developed by the Heart and Vascular service line.

“Our group chose the non-ST-segment-elevation myocardial infarction, or NSTEMI, in part because of the large number of patients it affects,” said Henry Weiner, M.D., FACC, associate section chief for quality and safety, Cardiology, at Christiana Care. “There are well recognized guidelines for therapy, but we have noticed a lot of variability in how we care for these patients. We thought there was an opportunity to improve care in this very large patient population.”
This year, Christiana Care has seen more than 850 heart attacks, and of those, 530 were NSTEMIs, as categorized by the patterns on an electrocardiogram.
“That’s about 50 a month,” Dr. Weiner said. “This clinical pathway is going to be used every day routinely at Christiana Care.”
Patients and providers first will experience the new pathway in the emergency room, where it is designed to expedite and improve diagnoses by increasing the amount of information provided to physicians early on.
In addition to administering an EKG, techs will be expected to employ a scoring system that predicts who is at a high risk to die or bleed and therefore should be taken first to the catheterization lab. The scoring system — known as thrombolysis in myocardial infarction, or TIMI — is classic, Dr. Weiner said, but hasn’t been used systematically because it is up to the provider. The process also will front-load the drawing of blood so that it is in the lab being tested for elevated troponins before a doctor consults with a patient.
Once a patient is diagnosed, the provider will be guided through the computerized drug ordering system by “hard” and “soft” stops.
“For example, if you don’t order a beta blocker, you won’t be able to proceed until you right-click on a contraindication,” Dr. Weiner explained. “It’s not a forcing function. If a doctor doesn’t want to start Mrs. Jones on a beta blocker, he doesn’t have to — but he has to explain his decision.”
The pathway also aims to improve patients’ experience and health outcomes by increasing their engagement in their own care. That will start in the hospital with education and sharing expectations.
“When I care for patients in general I try to orient them in terms of the course that they’re on and what the expected things are,” he said. “For example, I tell patients on day one or two after bypass surgery that they’ll turn the corner on day three or four.” The pathway will make it easier to help patients understand their individual plan of care.
Patients who follow up with cardiac rehabilitation fare better, but today only about two-thirds of patients do. A key post-discharge piece of the pathway will be trying to get patients engaged in rehab. At the suggestion of a patient adviser, the group also plans to start a support group for NSTEMI patients.
Currently, the pathway is planned to track patients for seven days post-discharge; ultimately the hope is to have enough resources in place to stretch that to a year.
The pathway’s success also will be gauged by the rate of utilization of the care pathway, readmission rates, mortality, length of stay and patient engagement.
One of the challenging pieces for providers will be getting used to the new computer programs.
“The system is going to be more directive, and that’s going to require some teaching and communication with providers so everybody understands where these changes have come from and how well they are grounded in therapy,” he said.
Ultimately, Dr. Weiner said, “What we hope is patients will spend less time in the emergency room, have a more coherent educational experience, and become more engaged in secondary prevention and the lifestyle modifications they need to make.”
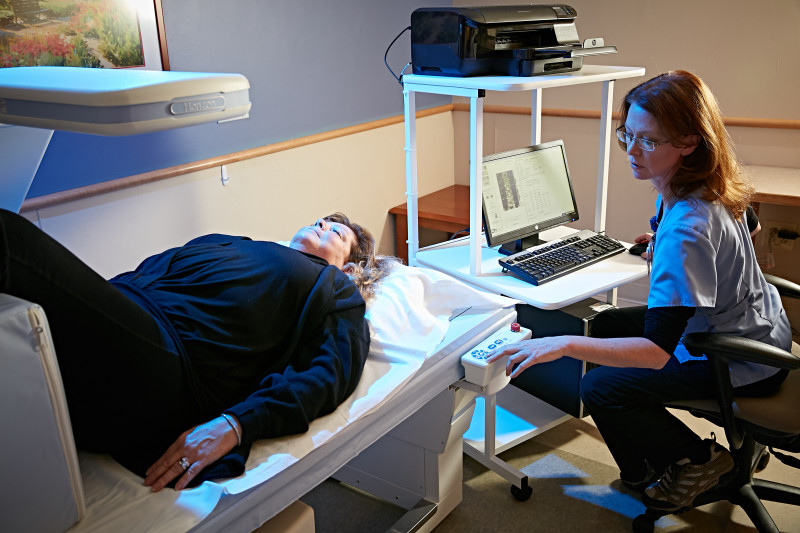
Musculoskeletal Health: Vertebral fragility fractures
The Musculoskeletal Health service line is using the clinical pathway effort to build on Christiana Care’s Strong Bones program, an initiative that already provides a system-based, consistent approach to evidence-based osteoporosis care.
The pathway will extend the program’s focus from hip and proximal humeral fractures to include vertebral fragility fractures.

“There’s a lot of variability in how vertebral fractures are managed,” said Eric Russell, D.O., a rheumatologist and associate physician leader for the service line. “There’s also inconsistent follow-up for post-fracture osteoporosis care. These are all things the pathway can help address by reducing variability in care and putting a focus on osteoporosis treatment to prevent further fractures.”
The pathway consists of two main components. The first is enhancing follow-up to ensure that patients are connected with an appropriate osteoporosis provider who can guide them through treatment to prevent future fractures. The second is to focus spine surgery consults to the minority who might benefit from it. Most patients will heal on their own and don’t require procedural intervention, he said, yet most are referred to a spine surgeon for an evaluation.
The pathway aims to enable optimal health and exceptional experience for patients by putting a new focus on outpatient osteoporosis treatment, including screenings and treatments to build up bone strength.

The program offers three resources to help patients meet that goal: a nurse navigator, a nurse practitioner and the Strong Bones network of osteoporosis providers.
The nurse navigator will be in touch with any patient who presents at Christiana Care with a vertebral fragility fracture to coordinate outpatient follow-up and bone-density scanning in preparation for seeing an osteoporosis doctor who ultimately will manage the patient’s care. For those admitted to the hospital, a nurse practitioner will consult with the patient to provide education, order appropriate lab testing and evaluate fall risks in concert with physical therapy. Together, they will help the patient navigate outpatient care.
“The pathway creates a new focus,” Dr. Russell said. “It gets our Strong Bones providers involved right up front.”
Through the Strong Bones referral network, primary care physicians may refer patients to osteoporosis providers for outpatient bone health management. Sports medicine, women’s health, rheumatology and endocrinology are all participating specialists in this program.
“We hope to see increased rates of early bone density screening and treatment and appropriate utilization of spine surgery consults,” Dr. Russell said. “The nurse navigator is really going to be a powerful tool in helping the patient navigate what needs to be done — anything from how to get a scan ordered, how soon to follow up with the doctor, to what to expect with treatment.”
The pathway has a technological component, too: Each patient will receive an automated discharge referral to the Strong Bones program along with a checklist of tasks to complete so that the patient becomes a partner in his own care. Russell said primary care doctors and osteoporosis specialists should experience improved coordination, with patients already having undergone fall precautions and appropriate lab work before they even show up for an office visit.
The pathway is expected to reach about 400 patients each year, and it will create a greater awareness of the importance of bone health.

Neurosciences: Acute ischemic stroke
As the only comprehensive stroke center in Delaware, Christiana Care ranks in the top 10 for stroke admissions in the country. Of those patients, about 80 percent have experienced an acute ischemic stroke, caused by an obstruction in a blood vessel supplying blood to the brain.
The prevalence of the condition, coupled with the robust resources Neurosciences already dedicates to strokes, made it a natural choice for the service line’s first clinical pathway.

M.D.
“Since we serve a large and complex group of stroke patients, we have a large opportunity to streamline care,” said Valerie Dechant, M.D., associate service line leader and medical director of Neuro Critical Care. In addition, the regulatory requirements the center already follows to earn accreditation provide existing data on the care of approximately 1,400 acute ischemic stroke patients served each year.
Like all of the clinical pathways, this one aims to reduce unnecessary variations in care, which also cuts down on avoidable costs.
“Every stroke patient who comes to Christiana Care will receive the same standard and quality of care, regardless of which physician is treating them or what nursing unit they’re on,” Dr. Dechant said.
The early focus of the effort will be on core clinical markers for which they have the best evidence, such as making sure the interdisciplinary team is engaged throughout a patient’s stay, and occupational and speech therapy is employed as appropriate. On discharge, that includes ensuring the patients are on the correct blood thinner and medicine to address risk factors like high cholesterol, and ensuring that case managers have devised a follow-up plan.
A core component to optimizing patients’ health outcomes and experience is heightening the level of patient education.
“We really want to involve them in their care,” said Melissa Bollinger, RN, BSN, MBA, operations leader for the service line and administrative director of Neurosciences.
That will involve communicating expectations and milestones to patients — and their family — that they can bring back to the provider.
“For example, they can say, ‘I should have had my CAT scan today.’ The key is that you incorporate the patient in the decision-making,” she said. “We want to make sure we communicate that we are standardizing the care but still providing individualized care.”
The team is rolling out the pathway and will ramp up in the spring and summer. They will assemble a patient and family focus group to help evaluate whether the effort is meeting patients’ needs.
“This is really a cultural change in the way we think of providing care to patients,” Bollinger said. “The clinical pathways are just the first step.”

Primary Care and Community Medicine: Type 2 diabetes
Primary Care and Community Medicine has chosen the farthest-reaching clinical pathway of all the service lines: the treatment of adults with Type 2 diabetes.

Choosing such a broad clinical pathway has several benefits, according to Omar Khan, M.D., MHS, FAAFP, physician leader for the Primary Care & Community Medicine service line. “One, it allows us to make a significant impact not only on this condition, but several associated chronic diseases,” he said.”As we build innovative ways to care for diabetics, the care of all patients is expected to improve. Second, it aligns many components of our large service line, which includes primary care specialties such as family medicine and internal medicine, medical subspecialties such as endocrinology and related support services such as nutrition services and diabetes education.”
Type 2 diabetes afflicts 70,000 people in Delaware, 25,000 of whom are seen at Christiana Care annually, said Amanda Klockars-McMullen, Ph.D., RN, CPHQ, program director for quality and performance improvement for Christiana Care Quality Partners and the Medical Group of Christiana Care, and project lead for the diabetes clinical pathway. More than 6 percent of Christiana Care’s own employees or their dependents are diabetic.
“The scope of this population is very broad. We also know it impacts not only health and well-being, but our utilization and costs,” she said. “In looking at our own data of how we care for patients, there was a wide variation. That’s why we wanted to create this pathway to standardize some of the delivery components.”
At the same time, the pathway will retain flexibility, particularly in educational materials for patients.
“For example, if you’re teaching what would be a healthy meal for Thanksgiving, it might look different from one culture or ethnicity to another,” she said. “We want to create the experience that’s most meaningful to patients.”
Also in that vein, the team plans to implement a variety of platforms for patients to choose to engage with their providers, including virtual visits, telehealth and shared appointments that provide education and a chance for peer bonding.
The innovation is being driven by the input of two focus groups of patient and family advisers.
“The feedback we heard very clearly was they wanted a peer support group so they would have somebody to call with questions,” Klockars-McMullen said.
The goal of the pathway will be to have the primary care and endocrinology practices work toward improving compliance and outcomes within the diabetes “metrics bundle,” which includes nine key care elements for diabetics, such as eye and foot exams, and HgA1c monitoring. In the longer term, it aims to reduce Emergency Department visits and hospital readmissions.
“We want to make sure patients are well controlled outside of the hospital,” she said.
The intent is to reduce variation among the practices in such areas as blood glucose control, medication management and office visit expectations. One simple adjustment was to make sure each practice had the equipment to perform an A1C test, used to gauge how a patient is managing the disease, said Margot Savoy, M.D., MPH, FAAFP, FABC, CPE, medical director, Department of Family & Community Medicine.
“There are disconnects between what providers know is available in the health system and how to access it,” Dr. Savoy said. “For example, some of the satellite practices didn’t know diabetes care coordinators were even an option.”
Staff will see the pathway reflected in a greater focus on teamwork. Each person who touches these patients will be provided a certain level of education about the disease so that everyone in the practice will be able to provide information, not just the physician.
Dr. Savoy said another shift will be toward employees working at the “top of their license” so they are playing a more valuable role than wasting time on inefficiencies below their skill set. From the patient’s perspective, that might mean seeing a change in who provides your care.
“Right now we have a lot of people doing work that they don’t need to be doing,” she said. For example, it’s appropriate for an endocrinologist to see a patient with difficulty controlling his diabetes. But the vast majority of patients with diabetes should be getting their diabetes care from their primary care physician.
“If the patient is truly stable, maybe they need to be seeing the nurse practitioner for the routine visits and checking in with the physician annually,” she said. “Our hope is you won’t feel like you’ve lost anything, but that you’ve gained a team. It should feel like care wrapped around and supporting the patient.”
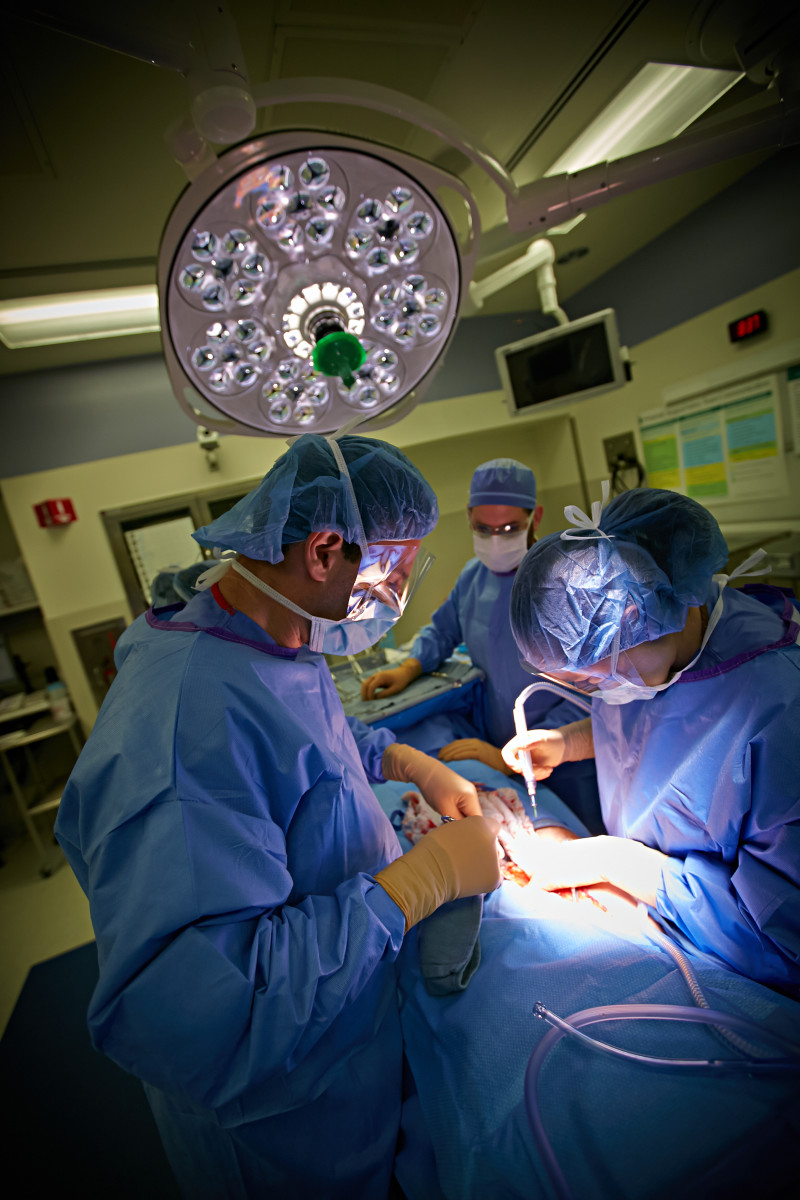
Surgical Services: Recurring ventral hernia abdominal wall reconstruction
Mark Schneider, M.D., MBA, has a whiteboard in his office where he is beginning to track the roughly 120 patients affected by recurring ventral hernia abdominal wall reconstruction, the focus of the Surgical Services clinical pathway.

“One of the reasons we chose this pathway is we are tracking every step these patients take,” said Dr. Schneider, chair of anesthesiology and associate service line leader for the Surgical Services service line. “Because of the complexity of these cases, we feel better tracking them end-to-end, and we’re learning from each patient.”
Patients undergoing this procedure have had multiple abdominal operations, Dr. Schneider explained. They have several incisions that don’t heal properly — perhaps due to diet, obesity, prior infection or recurrent hernias. The abdominal wall is so unhealthy it requires extensive repair.
The patients often are living with other health conditions such as sleep apnea or diabetes. They have a long length of hospital stay, about 7.5 days on average, and a prolonged recovery.
“It hit all the buttons of what we’re trying to do for all surgical patients,” Dr. Schneider said. “How do we optimize the co-morbidities? What can we do to standardize, where possible, the procedure itself? Is there any opportunity to provide more coordinated care that will result in a shorter hospital stay for the patient? And how can patients get back to work and daily activities?”
This clinical pathway will go far toward surfacing issues in coordination of care, he said. “We’re interested in taking this pathway and building a pathway for all surgical operations. Depending on the operation, it would use all or portions of it; it would be modified for each patient.”
One process the clinical pathway aims to change is how soon the care team becomes engaged with a patient.
“We are trying to stray from the idea that we only become aware of the patient when they become scheduled for surgery. We’re shifting that to when the surgeon says, ‘We think you are a candidate for surgery,’” he said. “As soon as they’re thinking about surgery, we can start looking at their health status, what resources they have at home and their level of awareness of what they need to do.”
That will require ongoing dialogue with patients, pre-op and post-op.
“The most interesting part is there will be better tracking of how patients recover, what things impact that recovery, so we can learn from that, and the next patient entering the system will have a better experience,” he said.
If the clinical pathway performs as designed, patients will be better prepared for surgery, experience fewer complications and be able to be released to a skilled nursing facility or return home.
Its success will be measured by a number of data points, including length of hospital stay, intensity of hospital resources required, complications, co-morbid conditions like deep vein thrombosis or the development of hyper- or hypoglycemia, and return visits to the Emergency Department.
“We noticed that some patients are returning within 30 days, and we’re looking into the reasons for that,” he said.
The pathway’s effectiveness also will be tracked on the patients’ end through surveys: How do they rate the level of care? Do they understand what they’re going through? Do they feel there is good communication with their providers?
As with the other service lines, this clinical pathway will rely on a multidisciplinary approach.
“We need everybody aware,” Dr. Schneider said. “These sorts of changes will take time.”
That includes the patient and his family, who must become partners in their health care.
“We’ll be giving them a checklist: This is what we need to accomplish,” he said. “We want the patient to own this checklist as much as the provider.”
That model has been shown to enhance recovery after surgery in the United States and Europe, he said.
“They literally give the patient a timeline and checklist: Look, if the nurse hasn’t come in and pulled out your drain by Thursday, you need to ask about it,” he said. “The pathway is laid out so everyone understands what’s supposed to be happening.”

Women’s and Children’s: Gestational diabetes
Nearly one-third of Delaware adults are classified as obese, the 17th highest ranking in the nation. With those statistics, it’s little surprise that Christiana Care is seeing more women with gestational diabetes, said Elizabeth Zadzielski, M.D., MBA, FACOG, medical director for ambulatory women’s health and associate Women’s and Children’s service line leader.
That’s one of the reasons the Women’s and Children’s service line chose the disease as the focus of its first clinical pathway.
“We also saw it as a way of bridging with our partners in Primary Care and Community Medicine,” who are addressing Type 2 diabetes in their pathway, she said.
Equally as important as early diagnosis and treatment in pregnancy is the follow-up care of gestational diabetes patients.

“These women have a significantly increased risk of becoming Type 2 diabetics within five years and are at a lifetime risk,” said Dr. Zadzielski. “We want to keep them informed after they’ve delivered and manage them appropriately, so should they become pregnant again, they’re in better shape.”
By reducing variations in care for women with gestational diabetes, the Women’s and Children’s service line also hopes to effect healthier outcomes for babies. Currently, 27 percent of children born to women with the gestational diabetes wind up in the neonatal intensive care unit.
“We want to see if by implementing a different model, we can have an impact on the NICU admission rate,” she said.
Like the other service lines, Women’s and Children’s will roll out its pathway gradually as the pieces come together. For example, down the road Dr. Zadzielski hopes to be able to equip patients with Bluetooth-enabled devices to record their blood sugar in real time.
“We’ve been relying on a paper-based record from patients. They do finger sticks and they write them down — it’s a very retrospective view,” she said. “What I would like to see happen is a device automatically feeding the blood sugar reading into the record.”
Patients and staff will see more immediate changes as the service line rethinks its model for delivering care. The current diagnostic process will be one of the first to be tweaked. Today, pregnant women who are not deemed to be at high risk for gestational diabetes are screened at 28 weeks with a one-hour test. If there is an abnormal result, they are sent for a three-hour diagnostic test. Sometimes, that means a lag of one or two months, if they go at all. Only about 75 percent of those who receive an abnormal result are following up with the longer test, Dr. Zadzielski said.
Instead, the service line will begin implementing a two-hour diagnostic test that will deliver results earlier in pregnancy.
“The patient goes in once, and they have to fast, and they have to be there for two hours, but you immediately get the diagnostic test,” she said.
Dr. Zadzielski expects the earlier diagnoses to double the patient population to about 400 women.
The clinical pathway also will focus on postpartum care. Only about 12 percent of women with gestational diabetes are following up with a screening test. The handoff to primary care partners will be critical, she said. That’s why she expects to join forces with endocrinologists and Family Medicine to create a more robust, coordinated educational system.
Also on the drawing board is the development of a gestational diabetes prenatal care group that could be offered in Spanish as well as English.
“That’s where we can really help educate a very vulnerable patient population,” she said.
Staff working with these patients can expect some re-education around the switch to the two-hour initial diagnostic test. Dr. Zadzielski will be looking for support to CareVio workers, who will make sure patients schedule the test and follow up with them if the results aren’t returned in a timely manner.
“Our goal is to improve outcomes for both mother and baby by working in closer collaboration with all of the members of our care delivery team,” she said.



